Family Decision Note
Choosing between a VA Community Living Center and private memory care involves complex eligibility, financial, and clinical considerations that depend on a veteran's service-connected status, disability rating, location, and bed availability. Benefit rules and copay amounts change periodically. Verify current eligibility and costs with a VA social worker, the VA Geriatrics and Extended Care office, or a VA-accredited representative before making final decisions. If private memory care is also on the table, consult an elder law attorney or financial planner familiar with VA benefits for the full financial picture.
Is a VA Community Living Center the same as a state veterans home, and which one would my father qualify for? That's the question I hear most often from families researching memory care for a veteran parent, and the honest answer is that the two aren't the same at all. A VA Community Living Center, usually called a CLC, is owned and operated directly by the Department of Veterans Affairs. A state veterans home is owned and operated by a state government, with the VA paying a per diem and certifying the facility each year. Different systems, different eligibility rules, different front doors. Private memory care is a third option entirely, with its own costs and its own trade-offs.
This confusion matters because it can send families down the wrong path for months. I've watched adult children spend weeks calling state veterans homes when the CLC at the nearby VA medical center would have been the better fit for their dad's situation, and the reverse happens just as often. The three options look similar on the surface. They aren't interchangeable underneath.
Imagine your father is a Vietnam-era veteran with service-connected dementia linked to a traumatic brain injury he sustained in combat. He's 78, his decline has accelerated over the past year, and you're comparing a VA Community Living Center forty minutes away with a private memory care community ten minutes from your home. Which one would he qualify for, what would each actually cost your family, and what are the honest trade-offs? That's what this article walks through.
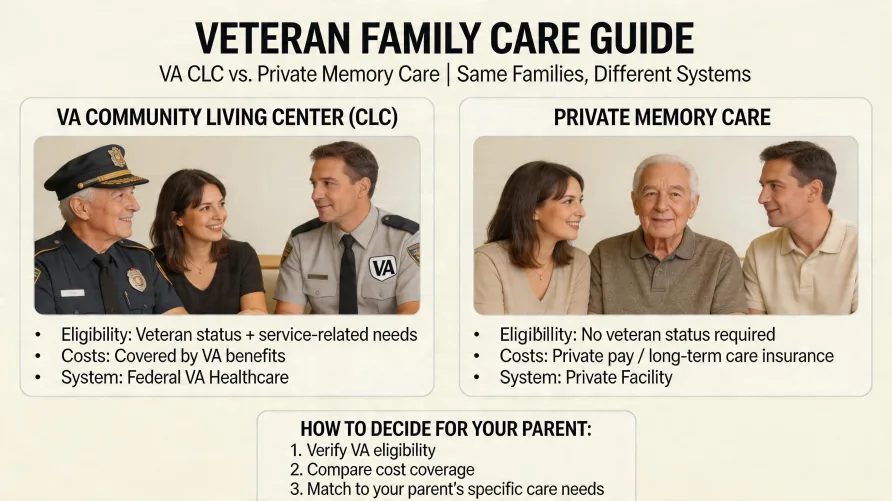
CLC vs Private Memory Care vs State Veterans Home: At a Glance
Before anything else, here's the comparison most families need to see first. The three care settings overlap in what they do but differ significantly in who runs them, who qualifies, and what they cost.
| Feature | VA Community Living Center (CLC) | Private Memory Care | State Veterans Home |
|---|---|---|---|
| Who owns/operates | Department of Veterans Affairs | Private company or nonprofit | State government (VA certifies) |
| Availability | ~130 locations nationwide | Thousands nationwide | At least one in all 50 states |
| Who qualifies | Enrolled VA health care, service-connected priority | Anyone who can pay | Varies by state, veteran status required |
| Monthly cost to family | $0 for most eligible veterans (copays possible) | $6,000 to $10,000+ | $0 to $3,500 (state-dependent) |
| Dementia care offered | Yes (in many locations) | Yes (specialized) | Yes (in many locations) |
| Length of stay | Short or long-term (clinical need) | Long-term, can be indefinite | Long-term typical |
| Primary access route | VA social worker + VA Form 10-10EC | Direct inquiry with community | State veterans agency application |
What a CLC Is, Who Qualifies, and How It Differs From State Veterans Homes
A VA Community Living Center is a nursing home that the VA owns, staffs, and runs directly. Most are located inside a wing of a VA medical center or on the same campus, which means residents have close access to VA physicians, specialists, and medication management that would be harder to coordinate from a private facility. The VA reports more than 100 CLC locations nationwide, and some senior-care sources place the current count closer to 130. None exist in Alaska, Rhode Island, Utah, or Vermont, so families in those states have to look to state veterans homes or community nursing homes instead. That geographic reality is one of the first things to check, because a CLC that's a four-hour drive from home isn't a practical long-term placement no matter how well-suited it is clinically.
CLCs provide both short-stay and long-stay services. Short-stay services include skilled nursing after a hospital discharge, rehabilitation, respite care, and hospice. Long-stay services include dementia care and continuing care for veterans whose functional needs exceed what home-based services can provide. Many CLCs run specialized dementia units with secured environments, behavior-focused staff training, and programming designed around the cognitive and emotional needs of veterans with Alzheimer's disease and related dementias.
Eligibility is where the CLC and state veterans home systems diverge sharply. To be considered for a CLC, your parent must first be enrolled in the VA health care system and medically and psychiatrically stable. Beyond that, the VA gives placement priority to three groups: veterans who need nursing home care for a service-connected disability, veterans with a combined service-connected disability rating of 70 percent or higher, and veterans with a total disability rating based on individual unemployability (TDIU). Veterans who don't meet these criteria may still receive CLC care if beds and resources are available, but they're not first in line, and placement often depends on income limits tied to the maximum VA pension rate with aid and attendance. The copay structure follows the same pattern. Long-term care is free for the first 21 days in any 12-month period, and starting on day 22 the copay runs up to $97 per day based on the financial information your parent provides on VA Form 10-10EC, the Application for Extended Care Services. Veterans with qualifying service-connected conditions are often exempt from copays entirely.
State veterans homes look similar from the outside but operate on a fundamentally different structure. The state owns and runs the facility. The VA certifies it annually and pays a per diem that offsets part of the cost of caring for each eligible veteran. Each state sets its own admission criteria, and some state homes will admit non-veteran spouses and Gold Star parents while a CLC won't. Geographic access is far broader because every state has at least one state veterans home, and some states have half a dozen or more. The trade-off is that you're coordinating with state bureaucracy rather than the VA directly, and the cost to your family varies more than it does at a CLC, ranging from near-zero in some states to a significant monthly payment in others.
During my years doing mobile X-ray inside rest homes and nursing facilities, I walked into plenty of buildings where the marketing materials and the day-to-day reality didn't match. That experience taught me to pay attention to what facilities feel like in the late afternoon when visiting family have gone home and the staffing gets thinner. CLCs have a different feel because the medical continuity with a VA hospital is right there, and the staff tend to be veteran-focused in a way that matters for residents with wartime trauma history. That's not a universal endorsement. CLCs vary in quality the way any large system does, and some have stronger dementia programming than others. The point is that the structural differences between these three options aren't cosmetic. They shape the care your parent will actually receive.
What Private Memory Care Offers That a CLC Doesn't Always
Private memory care communities are designed around cognitive care from the ground up. Most provide secured environments, staff trained specifically in dementia communication techniques, structured programming built around the progression of Alzheimer's and related dementias, and higher staff-to-resident ratios than you'll find in general nursing home settings. Families choosing private memory care usually value three things: location near family, a setting that feels more like a home than an institution, and flexibility around care levels as the disease progresses.
The catch is cost. National median monthly memory care rates run around $6,160 to $7,908 as of 2024-2025 data from the CareScout and Genworth Cost of Care Surveys, which works out to roughly $74,000 to $95,000 per year. States on the East Coast and West Coast often exceed $9,000 to $10,000 a month. That's where the financial shock hits families who haven't planned for it.
When a CLC Is the Right Answer, and When It Isn't
A CLC is usually the strongest fit for a veteran with a qualifying service-connected condition, a 70 percent or higher disability rating, or TDIU status, and especially for a veteran whose dementia or cognitive decline has a service-connected origin like traumatic brain injury, PTSD-related cognitive changes, or an Agent Orange presumptive condition. In those cases the CLC is not only free for the veteran but also delivers clinical continuity with a VA medical team that already has decades of records on the person. Families in this situation sometimes underestimate what they qualify for, assuming "VA care" just means the local outpatient clinic. It can mean much more than that, and the cost difference compared to private memory care is significant enough that it changes entire retirement plans.
Where the CLC falls short is geography and bed availability. With roughly 130 locations nationwide, most families don't have a CLC in their hometown. If the closest one is two hours away, regular family visits get hard, and for a person with dementia, the frequency of familiar faces is one of the things that most shapes quality of life. Long-term CLC placement also depends on available beds, and some CLCs focus more on short-stay rehabilitation than on dementia long-stay care. When a CLC is running near capacity, waits can extend out long enough that families bridge with private memory care or in-home care while they wait, which costs money the CLC route was supposed to save. My own family's experience with a dementia diagnosis drove home how quickly the timeline can compress, and how a placement decision that looked workable in January can become urgent by March.
A CLC also isn't always the right fit if your parent's identity and social needs aren't strongly tied to veteran status. Some veterans want to spend their final years around other veterans and appreciate the culture that comes with VA-run care. Others don't, and for them a private memory care community with people from more varied backgrounds can feel like a better match. That isn't a reason to dismiss CLC care, but it's worth weighing alongside the financial and clinical factors. Honest question: would your father feel more at home surrounded by other veterans, or in a mixed-community setting? Both answers are valid.
The other honest limitation is that a CLC is designed around clinical need rather than family preference. If your parent qualifies and a bed opens up, the VA expects the placement to happen. Declining a CLC placement in favor of private memory care can affect priority for future VA-funded care, so it isn't a decision to make lightly or reverse quickly.
Cost Comparison: The Real Math for Your Family
For a service-connected veteran with a 70 percent rating or higher who qualifies for a CLC, the annual cost to the family is often zero, with occasional copays after day 21 in any 12-month period. Compare that to private memory care at a national median of $7,500 a month, which runs $90,000 a year and often climbs past $120,000 annually in high-cost states. Over three years, that's a $270,000 to $360,000 difference. Over five, it can reach or exceed half a million dollars.
State veterans homes sit in between. With VA per diem support, monthly out-of-pocket costs for eligible veterans typically range from $0 to about $3,500 depending on the state. That adds up fast over time, but it's a meaningful savings over private memory care and often easier to access than a CLC because of broader geographic availability.
How to Apply for a VA Community Living Center Placement
The application path runs through the VA, not through the CLC directly. Your parent's VA primary care team, usually a VA social worker or case manager, initiates the process. The key forms are VA Form 10-10EC, the Application for Extended Care Services, which establishes copay status based on financial information, and VA Form 10-10172, the Community Care Provider Request for Service, which a VA physician or authorized private physician submits when nursing home level of care is clinically indicated. If your parent isn't enrolled in VA health care yet, enrollment is the first step, and compensation payments don't automatically equal enrollment. That catches a lot of families off guard.
Realistic timelines depend heavily on the local CLC's bed availability and your parent's priority group. For veterans with strong service-connected priority, placement can happen within weeks. For others, waits can extend months. Start the conversation with the VA social worker early, before a crisis forces a rushed decision.
A Decision Framework for VA CLC Memory Care vs Private Options
Rather than a scoring system, work through these practical questions as a family. Is your parent enrolled in VA health care, and if not, should enrollment start now regardless of which direction you go? What is your parent's current service-connected disability rating, and does the dementia or cognitive decline have a service-connected origin? How far is the nearest CLC from the family members who would visit most, and is that distance workable for weekly or biweekly visits?
Then turn to finances. What is the realistic monthly budget for care, including what Social Security, pension, and any savings can cover? If private memory care runs $7,500 to $10,000 monthly, how long can that budget sustain care before running out? Has anyone in the family spoken with a VA-accredited representative about which benefits your parent may qualify for beyond what you already know?
Finally, think about fit. Would your parent feel at home in a veteran-focused setting, or does a mixed-community environment match them better? Does the CLC you're considering have a strong dementia program, or is it mainly rehabilitation-focused with limited long-stay memory care capacity? These aren't questions with clean answers, but walking through them as a family surfaces the trade-offs that matter most.
Common Questions About CLC vs Private Memory Care
Does Medicare pay for a CLC? No. CLCs are funded by the VA system, not Medicare. However, Medicare may cover short-term skilled nursing at a private facility after a hospital stay, which is a different benefit entirely.
Can my parent use VA Aid and Attendance while living in a CLC? Generally no. Aid and Attendance is designed to reimburse out-of-pocket care costs, and a CLC is already VA-funded care. Veterans paying for private memory care or residing in a state veterans home with out-of-pocket costs may still qualify depending on their financial situation.
How long can my parent stay in a CLC? CLCs serve both short-stay and long-stay needs. For veterans with strong service-connected priority and ongoing clinical need, long-stay placement for dementia care is possible. For others, placements tend to be shorter and focused on rehabilitation.
Can a non-veteran spouse live with my parent at a CLC? No. CLCs serve veterans only. Some state veterans homes do admit non-veteran spouses and Gold Star parents, which is one of the practical differences between the two systems.
What if the nearest CLC doesn't have a dementia unit? Not every CLC runs a dedicated dementia long-stay program. Your VA social worker can identify which nearby CLCs offer specialized memory care and help you understand the alternatives, including Community Nursing Homes that contract with the VA.
Making the Call Between CLC and Private Memory Care
For most families of eligible service-connected veterans, a VA Community Living Center deserves a serious look before committing to private memory care. The financial picture is often dramatically different, and for veterans whose cognitive decline has a service-connected origin, the clinical continuity with an established VA medical team is a real advantage. The most common reason families don't pursue this route isn't that it's a worse fit. It's that nobody walked them through how the system actually works.
That doesn't mean a CLC is always the answer. Geographic distance matters. Cultural fit matters. Bed availability matters. If your parent wouldn't feel at home in a veteran-focused setting, or if the nearest CLC is too far from family, private memory care may be the right call even with the cost difference. There isn't one correct answer, only the right answer for your specific situation.
Start by calling the VA social worker assigned to your parent's care, or contacting the VA Geriatrics and Extended Care office at your nearest VA medical center. Ask about CLC capacity, dementia programming, and the realistic placement timeline for your parent's service-connected status. That single conversation often reshapes the rest of the decision. You don't have to figure this out alone, and the VA system has people whose job it is to help you sort through it.