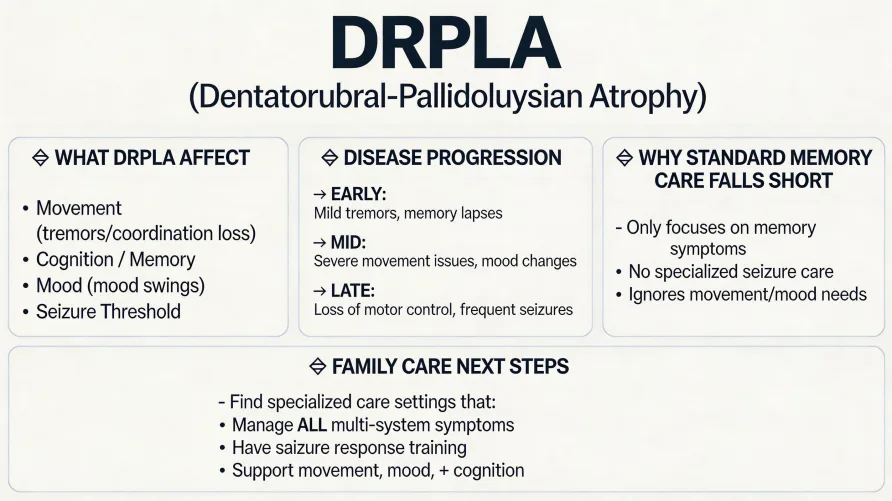
Dentatorubral-pallidoluysian atrophy (DRPLA) is a rare inherited brain disease caused by a genetic mutation in the ATN1 gene. It progressively damages areas of the brain that control movement, cognition, mood, and seizure threshold, creating care needs that extend well beyond what most memory care facilities are designed to handle.
Most families who end up researching DRPLA memory care have already been through years of uncertainty. Your parent's balance started declining. Personality shifts crept in. Maybe a neurologist diagnosed cerebellar ataxia while a psychiatrist treated the mood changes separately. Then a genetic test pulled everything into focus: DRPLA. You finally have a name for what your family has been managing, but you don't have a roadmap for what comes next.
That lack of a roadmap is the core challenge. DRPLA doesn't attack one system and leave the rest alone. It hits movement, cognition, emotional regulation, and seizure control at the same time, and those systems interact in ways that make care planning far more complicated than a typical dementia diagnosis. A fall-prevention plan has to account for both ataxia and involuntary choreiform movements. Medication for psychiatric symptoms has to be weighed against seizure thresholds. The staff watching your parent overnight needs to know what a DRPLA seizure looks like, not just how to redirect someone who is confused.
I've seen what happens when specialists treat their piece of the puzzle without talking to each other. During my years as a spousal caregiver, I spent more time relaying information between doctors than I did at home some weeks. That experience taught me something families dealing with DRPLA need to hear early: someone has to be the central hub, and in most cases, that person is you.
This article covers the key questions families ask once DRPLA enters the picture, from what the disease actually does to how you find a care setting equipped to handle it.
What Is DRPLA and How Does It Affect the Brain?
DRPLA stands for dentatorubral-pallidoluysian atrophy. The name refers to four specific brain structures that progressively deteriorate: the dentate nucleus and red nucleus (which coordinate movement), and the globus pallidus and subthalamic nucleus (which regulate motor control and behavior). The disease is caused by an abnormal expansion of CAG trinucleotide repeats in the ATN1 gene on chromosome 12. A healthy gene contains 6 to 35 repeats. People with DRPLA carry 48 or more.
DRPLA is autosomal dominant, which means a parent with the mutation has a 50% chance of passing it to each child. The disease also shows genetic anticipation: subsequent generations tend to develop symptoms earlier and more severely than the generation before them. That pattern catches families off guard. A grandparent may have shown mild ataxia in their 50s while a parent develops more pronounced symptoms decades sooner.
The condition is most common in Japanese populations, where it affects an estimated 2 to 7 per million people. Outside Japan, confirmed cases have been identified in families of European, African-American, and other ethnic backgrounds, though it remains extremely rare worldwide.
How Does DRPLA Progress Over Time?
DRPLA's progression depends heavily on the number of CAG repeats and the age when symptoms first appear. The average age of onset is around 31, but symptoms can begin anywhere from infancy to the early 70s. When the disease begins in adulthood (after age 20), the primary features are cerebellar ataxia, involuntary choreoathetoid movements, progressive dementia, and psychiatric disturbances including delusions and personality changes. No two patients look exactly alike, even within the same family.
The average disease duration is roughly 8 years from symptom onset, though some individuals live with the condition for much longer. Cognitive decline in adult-onset DRPLA often starts with executive function problems: difficulty planning, organizing, and following through on tasks that used to come naturally. Over time, the decline expands to affect memory, language, and daily decision-making. As the disease progresses, difficulty swallowing (dysphagia) becomes a serious concern, increasing the risk of aspiration pneumonia. That's a critical detail for care planning, because swallowing assessments need to be part of the ongoing care routine, not a one-time evaluation done at admission.
Managing DRPLA's Multi-System Impact in a Care Setting
This is where DRPLA breaks from the care model most memory care facilities are built around. Standard memory care is designed primarily for Alzheimer's disease and related dementias, with a focus on cognitive symptoms, wandering prevention, and behavioral redirection. DRPLA demands all of that plus active management of seizures, involuntary movements, psychiatric medication complexity, and progressive motor decline happening simultaneously.
Seizure Management in Memory Care
The question no one thinks to ask a memory care facility: does your staff know what to do when a resident has a seizure? Most memory care units focus on cognitive symptoms and wandering behavior. Seizure response protocols are common in hospitals and epilepsy centers, but they aren't standard in every residential care community. For a DRPLA resident, this gap can be dangerous.
DRPLA-related seizures in adults can include generalized tonic-clonic episodes, myoclonic jerks, and other seizure types that require staff who can recognize them quickly, position the resident safely, time the episode, and administer rescue medication if prescribed. Anti-seizure medications (ASMs) such as sodium valproate, levetiracetam, clobazam, and perampanel are commonly used to manage DRPLA-related epilepsy, often in combination. The medication regimen can be complex, and certain drugs like carbamazepine may actually worsen myoclonic episodes. Care staff need to understand not just when to give medication, but which medications interact with each other and what side effects to watch for.
Before placing a loved one with DRPLA in any facility, confirm whether direct care staff have completed seizure first aid certification (offered through the Epilepsy Foundation) and whether the facility maintains a written seizure action plan for each resident with a seizure disorder.
Chorea, Ataxia, and Fall Risk
The combination of cerebellar ataxia (impaired coordination and balance) and choreoathetosis (involuntary writhing and jerking movements) creates a fall risk profile that standard memory care environments aren't always prepared for. A resident with DRPLA doesn't just wander and get lost. Their body is working against them in ways that make every transfer from bed to wheelchair, every trip to the bathroom, a potential injury event. Physical therapy, adaptive equipment, and staff trained in safe transfer techniques for residents with movement disorders aren't optional for DRPLA care.
Psychiatric Symptoms and Medication Complexity
Psychiatric manifestations in DRPLA can include psychosis, delusions, hallucinations, aggression, and significant personality changes. These symptoms require psychotropic medications, but choosing the right ones is complicated. Some antipsychotics can worsen movement symptoms or lower seizure thresholds. The published literature on DRPLA is limited, but case reports have shown that atypical antipsychotics like quetiapine may be better tolerated than older antipsychotic drugs in these patients. The key takeaway for families: your parent's neurologist, psychiatrist, and primary care physician need to be communicating with each other and with the facility's medical director about every medication change.
During my years coordinating my husband's care across oncology, radiology, pain management, and primary care, I learned the hard way that specialists don't automatically share notes with each other. I spent evenings writing down what one doctor said so I could repeat it to the next. That coordination burden fell entirely on me, and it's the same burden DRPLA families face, often with even more specialists involved. This is why I recommend that families dealing with DRPLA seek out academic medical centers or neurology centers of excellence where multidisciplinary teams already work together. The coordination infrastructure exists in those settings. You shouldn't have to build it yourself.
What Should Families Ask a Memory Care Facility About DRPLA?
Walking into a memory care facility and asking about DRPLA will likely be met with blank stares. That's not a criticism of the staff. It's a reflection of how rare this disease is. The real question isn't whether they've heard of it, but whether they're willing and equipped to learn, adapt, and coordinate with your parent's medical team.
Ask whether the facility has experience caring for residents with active seizure disorders, not just dementia. Ask who on staff is trained in seizure first aid, and how often that training is refreshed. Ask how they handle residents with involuntary movement disorders and what fall-prevention protocols look like beyond bed alarms. Ask whether there is a nurse on-site 24 hours a day (not just on call) and whether the facility's medical director is willing to coordinate directly with outside neurologists and psychiatrists. Ask about medication administration procedures for complex multi-drug regimens.
I've visited care facilities during my years doing mobile X-ray work, and the gap between what a brochure promises and what actually happens on the floor at 2 a.m. can be wide. Get specific answers, not reassurances.
Can Standard Memory Care Handle DRPLA's Needs?
Some can. Most can't, at least not without significant customization. Standard memory care is built for a resident whose primary challenge is cognitive decline, confusion, and behavioral symptoms related to Alzheimer's or a similar dementia. DRPLA adds layers of medical complexity that push beyond that framework.
The most realistic options for many families fall into a few categories. A memory care facility with a strong nursing staff, an on-site medical director, and willingness to work closely with a neurology team may be able to provide appropriate care with the right plan in place. A skilled nursing facility with a dedicated memory care wing may offer more medical infrastructure, though the environment may feel less residential. For families near academic medical centers, outpatient neurology partnerships can supplement a residential placement.
There's no perfect answer here. The right fit depends on which symptoms are most prominent at the time of placement and how quickly the disease is progressing.
How Much Does DRPLA Memory Care Cost?
Memory care costs vary widely by location and level of care, but families should plan around a national median of roughly $6,700 to $8,000 per month as of 2025. That translates to approximately $80,000 to $96,000 per year. Over a multi-year stay, the total can climb well past $200,000, and DRPLA's medical complexity can push costs even higher if the facility charges additional fees for residents with active seizure disorders or complex medication needs.
Medicare does not cover memory care. Medicaid may help in some states, but coverage varies and waitlists are common. Long-term care insurance, if your parent purchased a policy before diagnosis, may cover a portion. The financial shock is real. When my own family faced memory care costs for a loved one with dementia, the numbers hit harder than any of us expected, even though we thought we'd planned ahead.
What Role Does Genetic Counseling Play for DRPLA Families?
Because DRPLA is autosomal dominant, genetic counseling isn't just recommended. It's essential for the broader family. Each child of an affected parent has a 50% chance of carrying the expanded ATN1 gene. Genetic anticipation means that children who inherit the mutation may develop symptoms earlier than their parent did, potentially with more severe features.
Genetic testing is available through specialized laboratories, and a genetic counselor can help family members understand the implications of testing, including the emotional weight of learning your own risk status. For families already caring for a parent with DRPLA, the question of whether to test adult children often comes up during care planning discussions. This is a deeply personal decision, and there is no single right answer. Some family members want to know so they can plan financially and medically. Others choose not to test. Both decisions are valid. A qualified genetic counselor can guide that conversation without pressure.
Finding Your Family's Path Forward
DRPLA is one of the rarest diagnoses a family can face, and the care planning that follows is unlike anything most memory care resources prepare you for. The disease doesn't follow the patterns that most facilities, most insurance systems, and most family expectations are built around. That can feel isolating.
But families manage it. They find neurologists who specialize in ataxias and movement disorders. They ask hard questions of care facilities and hold them to specific answers. They build coordination systems between specialists because that's what the disease demands.
Start with a neurologist connected to a comprehensive ataxia or movement disorder center. Build your care team before you need a placement, not during a crisis. And remember that asking for help coordinating all of this isn't a sign that you're failing. It's a sign that you understand what your family is up against, and that you're doing exactly what your parent needs you to do.