Most families learn this the hard way. When a urinary tract infection hits a younger person, the symptoms are obvious: burning, urgency, frequent trips to the bathroom. But when a recurrent UTI hits your elderly parent, those classic signs often don't show up at all. Instead, the first clue is something far more alarming. Your parent becomes suddenly confused, agitated, or disoriented, and you rush to the ER convinced it's a stroke or the beginning of dementia.
I've seen this play out hundreds of times in the emergency room. A family brings in their parent, terrified that something catastrophic has happened to their brain. And more often than I can count, the answer comes back from a simple urinalysis, not a brain scan. It's a urinary tract infection.
Recurrent UTIs in elderly adults are one of the most underrecognized triggers for confusion, falls, and ER visits. For families watching a parent cycle through repeated episodes of sudden disorientation, the connection between a bladder infection and cognitive changes can be the missing piece they've been searching for. Understanding this link doesn't just change how you respond in the moment. It can change the entire care plan, including whether your parent needs a level of daily supervision that home care alone can't provide.
This article covers why UTIs behave so differently in seniors, how recurrent infections create a dangerous cycle, and the prevention strategies and care environments that can break that pattern.
How Recurrent UTIs Present Differently in Seniors
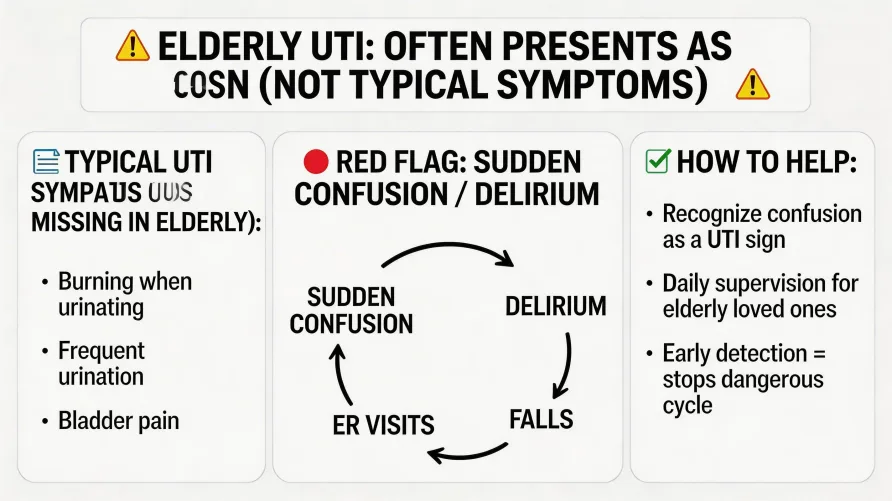
In younger adults, a UTI announces itself clearly. There's pain during urination, a constant urge to go, and sometimes blood in the urine. In seniors, those symptoms may be entirely absent. Research published in the journal Cureus found that UTIs in elderly patients commonly present as delirium, confusion, drowsiness, falls, and loss of appetite, often without any fever. The infection is there, but it's hiding behind symptoms that look like something else entirely.
This atypical presentation is what makes UTIs in elderly adults so dangerous. Families see the confusion and assume the worst. Doctors who aren't looking for a UTI may order brain imaging before checking the urine. The behavioral changes can include agitation, withdrawal, hallucinations, or a sudden inability to follow conversations. If your parent has existing cognitive decline, a UTI can make it look like their dementia has suddenly gotten much worse overnight.
The key distinction is speed. Dementia progresses gradually over months and years. UTI-related delirium comes on within hours or days. That sudden onset is the red flag every family should know.
The UTI-Confusion Connection: What Every Family Should Know
The link between urinary tract infections and sudden confusion in elderly adults isn't a vague association. It's a well-documented medical phenomenon with a specific biological mechanism behind it. When bacteria infect the urinary tract, the body mounts an immune response that releases inflammatory proteins into the bloodstream. In younger people, the brain can handle that inflammatory load without much disruption. In older adults, the brain is more vulnerable. The blood-brain barrier becomes more permeable with age, and those inflammatory signals can directly interfere with how neurons communicate, producing the disorientation, memory lapses, and behavioral changes that define delirium.
Research from Cedars-Sinai has identified a specific inflammatory protein, interleukin-6 (IL-6), as a key driver of UTI-related delirium. In laboratory studies, blocking this protein reversed the delirium-like symptoms entirely. This matters because it confirms that the confusion isn't a sign of permanent brain damage. It's a reversible response to infection, and once the UTI is treated, most patients show significant improvement within 24 to 72 hours.
But here's what families often underestimate. In elderly patients, UTIs don't cause the typical burning or urgency that would send a younger person straight to the doctor. The first sign is often sudden confusion that looks exactly like dementia. A parent who was lucid yesterday may not recognize where they are today. They may become combative with caregivers, pull at their clothing, refuse food, or become convinced that strangers are in the house. Some parents become unusually drowsy and withdrawn. Others swing in the opposite direction, growing restless and pacing at odd hours. The range of behavioral changes is wide, which is part of why the infection gets missed so often. These aren't personality changes or signs of rapid cognitive decline. They're symptoms of an infection that a simple urine test can identify, and families who don't know this connection can spend months chasing a dementia diagnosis that delays the treatment their parent actually needs.
The pattern families should watch for is telling. A parent who experiences sudden confusion, gets treated for a UTI and improves, then declines again a few weeks later may be caught in a recurrence cycle. Recurrent UTIs are defined as two or more infections in six months or at least three within a year, and they're twice as common in women over 65 as in the general population. Risk factors include incomplete bladder emptying, postmenopausal estrogen loss, diabetes, catheter use, dehydration, and incontinence. Each of these becomes more common with age, which is why the recurrence rate climbs so steeply in older adults.
I learned early in my career that when a senior comes into the ER with sudden-onset confusion, the smartest first step is checking the urinalysis before jumping to neurological workups. That instinct has saved countless patients from unnecessary imaging, delayed treatment, and the fear that comes with a suspected stroke or rapid dementia progression. Families can apply the same thinking at home. If your parent's mental state changes abruptly, a UTI should be the first thing you rule out, not the last.
The danger of missing this connection goes beyond the individual episode. Prolonged or severe delirium in elderly patients is associated with longer hospital stays, accelerated cognitive decline, and increased short-term mortality. Getting a UTI diagnosed and treated quickly isn't just about resolving the current confusion. It's about protecting your parent's long-term brain health.
The Dangerous Cycle: Infection, Confusion, and Falls
Recurrent UTIs don't just cause confusion. They create a cascading cycle that puts your parent at serious physical risk. The sequence is predictable: a UTI triggers delirium, the confusion leads to unsteady movement or poor judgment, and a fall follows. Falls are the leading cause of injury-related death among adults 65 and older, and the CDC reports roughly one million fall-related hospitalizations each year among older adults. When a UTI is quietly driving the confusion behind those falls, the cycle repeats until someone identifies the root cause.
Consider a situation where your parent becomes suddenly confused and agitated in the middle of the night. The family rushes to the ER, fearing a stroke or dementia onset. The diagnosis comes back as a urinary tract infection. Antibiotics resolve the confusion within a couple of days, and everyone exhales. Then it happens again six weeks later. And again after that. By the third episode, the family starts to see the pattern: UTI causes confusion, confusion causes falls or near-falls, and the ER visits keep stacking up. That's the point where many families realize something about the daily care environment has to change.
Risk Factors That Make Recurrent UTIs More Likely
Understanding why your parent keeps getting UTIs is the first step toward breaking the cycle. Several age-related changes increase susceptibility. In women, declining estrogen levels after menopause thin the vaginal and urethral tissues, making bacterial colonization easier. In men, prostate enlargement can prevent complete bladder emptying, creating a breeding ground for bacteria. Diabetes, which impairs immune function, is a well-established risk factor for both initial and recurrent UTIs.
Dehydration is one of the most preventable risk factors, and one of the most common. Many older adults drink less because they worry about incontinence or simply lose the sensation of thirst. Incontinence itself creates a vicious circle: moisture and bacterial exposure from wet undergarments increase UTI risk, while the UTI worsens the incontinence. Cognitive decline adds another layer, because a parent who can't remember to drink water or maintain personal hygiene is at far higher risk.
Catheter use carries its own significant risk. According to the CDC, about 75% of UTIs acquired in hospitals are associated with urinary catheters, and each day a catheter remains in place adds a 3% to 7% increased risk of infection. For parents discharged home with a catheter, the risk of recurrent infection is substantial unless someone is providing consistent daily care. Without monitoring, these risk factors go unmanaged until a crisis hits.
UTI Prevention Strategies That Actually Work
Prevention starts with the basics, but the basics require consistency that many elderly adults living alone can't maintain. Adequate hydration is the single most important preventive measure. Drinking enough water throughout the day helps flush bacteria from the urinary tract before infection can take hold. The challenge is that many seniors need reminders and encouragement to drink, especially those with cognitive decline who may forget or resist.
Hygiene protocols matter, particularly for women. Proper bathroom hygiene, regular clothing changes, and prompt attention to incontinence all reduce bacterial exposure. For postmenopausal women, vaginal estrogen therapy has shown strong results in clinical studies, reducing recurrent UTIs by restoring the protective vaginal flora that declines after menopause. This is a conversation worth having with your parent's doctor if infections keep recurring.
For parents with catheters, the goal should always be to minimize catheter use and remove the device as soon as it's no longer medically necessary. When a catheter is required, proper care and regular replacement following medical guidelines can significantly reduce infection risk. These aren't complicated strategies, but they require someone paying attention every day. That's the piece that breaks down when a parent is living without adequate supervision.
When Recurrent UTIs Signal the Need for Supervised Care
A single UTI is a medical event. Recurrent UTIs are a pattern, and that pattern often reveals a gap in daily care that families can't always fill from a distance. If your parent keeps getting infections because they aren't drinking enough water, aren't maintaining hygiene, or aren't getting to the bathroom safely, those are supervision problems, not just medical ones.
Having watched a family member's health decline, I know exactly how this realization hits. When someone you love starts cycling through confusion episodes, your first instinct is to keep managing from the sidelines, calling more often, stopping by on weekends, hoping the pattern will break on its own. But the infections kept coming, and each one chipped away at a little more of who she was. The gap between what she needed every day and what the family could provide from a distance became impossible to ignore. That experience taught me that recognizing the need for supervised care isn't giving up. It's acting on what you can see clearly, even when it hurts.
Ask yourself candidly: Is your parent drinking enough fluids on their own? Can they maintain personal hygiene independently? Does someone notice behavioral changes quickly enough to catch a UTI before it escalates? Can they get to the bathroom safely at night? If the answer to most of these is no, it may be time to evaluate senior living options that provide daily oversight.
What to Look for in a Senior Living Community for UTI-Prone Residents
Not all senior living communities handle recurrent UTIs with the same level of attention. When touring facilities, ask specifically about how staff monitor hydration, their protocols for tracking and responding to behavioral changes, and how quickly they can arrange urinalysis when a resident shows signs of confusion. Communities with trained nursing staff on-site can catch UTIs earlier than family members checking in by phone.
Ask about their approach to catheter management if your parent uses one. Find out whether they have established relationships with physicians or nurse practitioners who understand the UTI-delirium connection in elderly residents. A facility that tracks infection patterns and adjusts prevention strategies for individual residents demonstrates the kind of proactive care that can break the recurrence cycle. During my mobile X-ray work visiting care facilities, I saw wide variation in how attentive staff were to these details. The difference between a facility that catches a UTI on day one and one that waits until a resident falls is the difference between a routine course of antibiotics and a hospital admission.
Taking the Next Step for Your Parent
Recurrent UTIs in elderly parents are more than a nuisance. They're a medical pattern with real consequences: repeated delirium episodes, increased fall risk, ER visits, and potential long-term cognitive impact. The good news is that this pattern is recognizable, treatable, and often preventable with the right level of daily care.
If your parent has been cycling through confusion episodes that turn out to be UTIs, you now understand the mechanism behind that connection and the prevention strategies that can help. You also know the honest question to sit with: is your parent getting the consistent daily supervision needed to prevent these infections and catch them early when they do occur?
There's no perfect answer, and every family's situation is different. But understanding the link between recurrent UTIs and the care environment is a powerful starting point. You're not failing your parent by recognizing they need more help. You're protecting them.