Posterior cortical atrophy is one of the most commonly misdiagnosed forms of Alzheimer's disease, with families waiting a median of three years between the first symptoms and a correct diagnosis. A 2025 Mayo Clinic study of more than 500 people with PCA found that nearly half saw an eye doctor before anyone considered a neurological cause, and roughly a third of those patients underwent unnecessary eye procedures, including cataract surgeries and LASIK, before a neurologist identified the real problem. For families already watching a parent struggle, those lost years carry real consequences.
Imagine your mother keeps bumping into furniture, misjudging the depth of stairs, and recently stopped driving after several close calls in parking lots. You take her to an ophthalmologist. The exam comes back normal. You try a second eye doctor, then a third. Her glasses prescription barely changes. Nobody can explain why she reaches past her coffee cup or flinches at shadows on the floor. It isn't until a neurologist orders brain imaging that someone finally explains: her eyes work fine, but her brain can no longer process what they see.
That pattern is far more common than most families realize. From my own experience with a family member's cognitive decline, I know how disorienting it is when symptoms don't match what you expect dementia to look like. We kept thinking the vision issues were separate from everything else. They weren't.
This article explains what posterior cortical atrophy is, why it's classified as Alzheimer's disease despite looking nothing like it, and what families should look for in a memory care environment designed to support someone with visual-processing deficits.
What Is Posterior Cortical Atrophy?
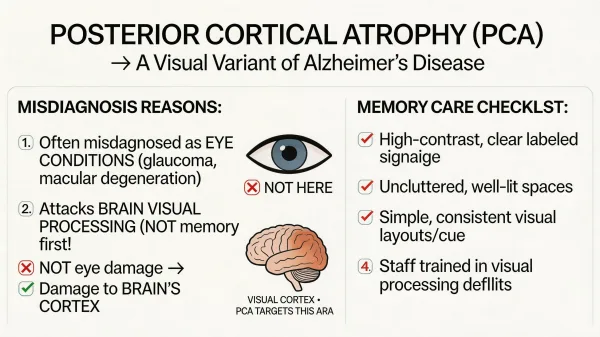
Posterior cortical atrophy (PCA) is a neurodegenerative syndrome that damages the back of the brain, the region responsible for processing visual information. Unlike typical Alzheimer's, which attacks memory centers first, PCA targets the parietal and occipital lobes, causing progressive loss of the ability to interpret what the eyes see. Memory often stays relatively intact in the early stages, which is exactly why it gets missed.
Common early symptoms include difficulty reading (words seem to move on the page), trouble judging distances, problems recognizing familiar faces, getting lost in known spaces, and struggling with tasks that require hand-eye coordination like pouring water into a glass. Most people develop symptoms between ages 50 and 65, younger than typical Alzheimer's. That younger onset adds another layer of confusion, because families and even doctors aren't expecting a degenerative brain disease in someone in their late fifties.
Where This Gets Confusing: Eyes vs. Brain
The core problem with PCA diagnosis is that it looks like an eye problem. The person can't read, can't judge distances, can't find objects sitting right in front of them. Every instinct says to see an eye doctor. And the eye doctor runs tests that come back normal, because the eyes themselves are fine. The issue is cortical: the visual cortex and surrounding brain regions are atrophying, so the brain can't assemble a coherent picture from the signals the eyes are sending.
This is where I wish our family had known more. When a family member started having trouble with depth perception and reading, we spent months chasing ophthalmology appointments. Each time, we were told the eyes looked healthy, maybe a slight prescription change. Nobody mentioned the possibility that a brain condition could cause visual symptoms while leaving the eyes untouched. By the time we got to a neurologist, the disease had progressed further than it needed to. That delay didn't just cost us time for planning. It cost us time with the person we knew. Looking back, the signs were there early, the way she'd hesitate at curbs, the way familiar rooms suddenly seemed hard to move through. We just didn't know what we were looking at. If your parent's vision problems don't improve with new glasses and eye exams keep coming back clean, push for a referral to a neurologist who can evaluate cortical function. That single step can change the entire trajectory of your family's care planning.
The typical PCA patient sees two or three eye specialists over one to three years before someone orders brain imaging. That window matters. Early diagnosis doesn't change the disease course, but it gives families time to plan, to set up power of attorney, to research care environments before a crisis forces a rushed decision.
Why PCA Is Still Alzheimer's Disease
Families often ask how something that looks like a vision disorder can be Alzheimer's. The answer is in the underlying pathology. A 2024 international meta-analysis published in The Lancet Neurology examined autopsy data from 145 people diagnosed with PCA and found that 94% had Alzheimer's disease as the primary pathology. The same amyloid plaques and neurofibrillary tangles that define Alzheimer's are present, just concentrated in the back of the brain rather than the hippocampus (the memory center). The Alzheimer's Association estimates that PCA accounts for about 5% of Alzheimer's cases seen in memory clinics, though the actual percentage may be higher because so many cases go unrecognized.
As PCA progresses, memory, language, and executive function do decline. Late-stage PCA eventually resembles advanced typical Alzheimer's. The distinction matters most in the early and middle stages, when the person's needs are driven by visual and spatial deficits rather than memory loss, and the care environment needs to reflect that difference.
How Posterior Cortical Atrophy Memory Care Environments Should Be Designed
Standard memory care is built around memory loss: locked doors to prevent wandering, name-labeled rooms, routine-based schedules. Those features still matter for PCA, but they aren't enough. A person with PCA needs an environment designed around visual-processing deficits, and most families don't realize how specific that design needs to be until they start touring facilities.
Contrast is the foundation. When the brain struggles to distinguish objects from their backgrounds, color contrast becomes a safety tool. Toilet seats should be a distinctly different color from the floor and walls. Handrails need to stand out from the wall surface. Doorframes, light switches, and grab bars should all contrast sharply with surrounding surfaces. I've been inside facilities during mobile X-ray work where everything was the same shade of beige, walls, floors, handrails, door handles. For a resident with PCA, that kind of environment is functionally invisible. They can't see where the wall ends and the door begins.
Clutter is a serious problem for PCA residents. Research from University College London has shown that visual clutter disproportionately affects people with PCA compared to those with typical Alzheimer's. When a table is covered with magazines, cups, napkins, and utensils, a PCA resident may not be able to locate any single item. The brain can't separate individual objects from the visual noise. Care environments need to be intentionally sparse: clear tabletops, minimal decorations on walls, uncluttered hallways. This feels counterintuitive to many families who want a warm, homelike setting, but for PCA, simplicity is safety.
Lighting requires careful attention at every level. Overhead fluorescent lighting creates glare on shiny floors, which a PCA resident may interpret as a wet surface or a change in floor level. Shadows cast by uneven lighting can look like steps or holes. The best environments use consistent, diffused lighting that minimizes both glare and stark shadow lines. Natural light helps during the day, but windows need treatments that prevent bright patches of sun from creating disorienting contrast against darker interior spaces. Lights should be on before dusk rather than switched on after it gets dark, because the transition period is when visual confusion peaks.
Fall prevention in PCA goes beyond non-slip flooring. Depth-perception deficits mean a resident may not see a step that's right in front of them, especially if the step and the floor are similar in color. Stair edges need high-contrast striping. Transitions between flooring materials (carpet to tile, for example) should be flush and similar in tone. Dark mats on light floors look like holes to a PCA resident and can cause freezing or falling. Patterned flooring, especially geometric or high-contrast patterns, can create the illusion of uneven surfaces and should be avoided entirely.
Standard memory care signage is designed for people who can still read and recognize symbols. That assumption breaks down with PCA. Residents may not be able to read a sign, recognize a pictogram, or even perceive a sign as distinct from the wall behind it. Color-coded pathways (a blue stripe leading to the dining room, a green stripe to the bedroom wing) work better than text-based wayfinding for PCA residents. Large-format personal photos on bedroom doors help more than name plates. Any wayfinding system that relies on reading or symbol recognition will fail as PCA progresses, so the environment itself needs to do the guiding through color, texture, and spatial layout.
What to Ask When Touring a Memory Care Facility
Not every memory care community understands PCA, and that's something you can assess during a tour. Ask directly whether the facility has cared for residents with posterior cortical atrophy or other visual-variant dementias. Pay attention to the answers.
Look at the physical environment yourself. Are hallways cluttered with carts and equipment? Is the flooring a uniform color, or does it have patterns that could confuse someone with depth-perception problems? Do bathroom fixtures contrast with walls and floors? Is the lighting even, or are there bright spots and dark corners? These aren't cosmetic preferences. For a PCA resident, they're the difference between being able to find the bathroom independently and needing a staff member for every move.
Ask about staff training on visual-processing deficits. Staff accustomed to memory-led dementia may interpret a PCA resident's behavior as confusion or non-compliance when it's actually a visual-processing failure. A resident who won't sit down may not be refusing. They may not be able to see the chair. That distinction changes everything about how care is delivered. In my years working in hospital settings, I've seen how quickly staff assumptions can shape a patient's experience, and the wrong assumption about someone with PCA can lead to frustration on both sides.
Planning Ahead After a PCA Diagnosis
A PCA diagnosis can feel isolating, partly because so few people have heard of it and partly because the symptoms don't fit the story most families expect from Alzheimer's. Your parent may still remember your name, your birthday, your childhood stories, and yet can't pour a glass of water without missing the cup. That contrast is jarring, and it's okay to find it confusing.
The right memory care environment won't stop the progression of PCA, but it can preserve your parent's independence and dignity for longer than an environment that wasn't designed with their specific needs in mind. Start looking at facilities before you're in crisis mode. Ask the hard questions about contrast, lighting, clutter, and staff training. Trust what you see during tours more than what you read in brochures.
You're already doing something important by learning about this condition. The families who understand what PCA is and what it requires are the ones best positioned to find care that actually fits.