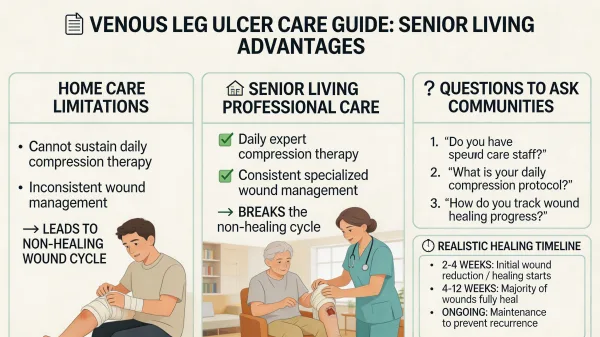
When a Wound Won't Heal: Understanding Venous Leg Ulcers
If your parent has an open wound on their lower leg that has been there for weeks or months without improving, you already know the frustration. The dressing changes, the home health visits, the slow realization that what you're doing isn't working. Venous leg ulcers are among the most common chronic wounds in older adults, affecting an estimated 1% to 3% of adults in the U.S. and climbing higher, up to 4% or more, in people over 65. They're also among the most stubborn wounds to heal.
Here's what most families don't realize early enough: venous leg ulcers won't heal without consistent, properly applied compression therapy and daily wound management. Twice-a-week home health visits, while helpful, often aren't enough to break the cycle. The wound needs daily assessment, daily dressing changes, and steady compression to give the tissue underneath a real chance to recover.
I learned during my years as a spousal caregiver that consistency is the difference between a wound that heals and one that gets worse. One skipped dressing change can erase a week of progress.
This article covers what venous leg ulcers are, why they resist healing in home settings, what proper compression therapy looks like, and how to evaluate whether a senior living community can provide the daily wound management your parent needs. You'll also find honest information about healing timelines, costs, and what to expect after the ulcer closes. If you've been watching a wound get worse instead of better, the right care environment can change the trajectory.
What Are Venous Leg Ulcers and Why Do They Develop?
A venous leg ulcer is an open wound on the lower leg, typically near the ankle, caused by chronic venous insufficiency. In a healthy circulatory system, one-way valves inside the leg veins push blood back up toward the heart. When those valves weaken or fail, blood pools in the lower legs, creating sustained high pressure in the veins. Over time, that pressure damages the surrounding skin and tissue until an open wound forms.
Venous ulcers account for roughly 70% of all chronic leg ulcers and affect an estimated 1% to 3% of the general adult population. That number climbs to around 4% for adults over age 65, according to research published in the Journal of the American Academy of Dermatology. The ulcers typically appear as shallow, irregular wounds with well-defined edges, often surrounded by discolored, hardened skin. They can range from small and manageable to large and painful, and without treatment, they tend to grow rather than shrink.
The key thing to understand: the wound itself is a symptom of an underlying circulation problem. Treating the wound alone without addressing the venous pressure beneath it is like mopping a floor while the faucet is still running. This is why basic wound care, cleaning and bandaging without compression, rarely resolves a venous ulcer. The pressure in the veins keeps damaging new tissue as fast as the body can repair it.
Why Venous Ulcers Don't Heal at Home: The Compression Therapy Gap
Compression therapy is the single most important treatment for venous leg ulcers. Research consistently shows that wounds treated with proper compression heal significantly faster than those without it. A Cochrane review found that patients receiving compression therapy were nearly twice as likely to heal compared to those who received standard care without compression. The principle is simple: external pressure applied to the lower leg counteracts the internal venous pressure that caused the ulcer in the first place. That pressure reduces swelling, improves blood flow back toward the heart, and creates the conditions tissue needs to rebuild itself.
But here's where home care often breaks down. Effective compression isn't something you can manage casually. Multi-layer compression bandaging, the approach that clinical evidence supports most strongly, requires a trained professional to apply it correctly. The bandages need to deliver specific pressure levels, typically between 25 and 40 mmHg at the ankle, and they need to be reapplied with each dressing change. Too little pressure and the therapy doesn't work. Too much pressure and you risk cutting off arterial blood flow, which can cause serious harm. This is especially critical for older adults who may have mixed arterial and venous disease, where an ankle-brachial pressure index test must confirm adequate arterial circulation before any compression is applied.
In most home health setups, a nurse visits one to three times per week. Between those visits, the wound may go a full day or two without a proper assessment. Dressings may shift, get wet, or lose their compression. The patient may not elevate their leg enough. Small changes in the wound, early signs of infection like increasing redness, warmth, new pain, or changes in drainage color, go unnoticed for days. I've seen in my own caregiving experience how quickly a wound can go backward. You do everything right for five days, miss one dressing change, and the wound looks worse than it did the week before. That kind of setback is demoralizing for everyone involved.
Consider a situation where your parent has had an open wound on their lower leg for six months. Home health sends a wound care nurse twice a week, but between visits, your parent struggles to keep the dressing clean and intact. The wound has gradually gotten larger rather than smaller, and the surrounding skin is becoming more discolored and tender. This is a common pattern, and it doesn't mean you or the home health team failed. It means the wound needs more consistent care than a twice-weekly visit can provide.
When I was caring for my first husband through his cancer treatment, I managed feeding tubes, dressings, and wound sites every single day for years. What that experience taught me is that wound care isn't just about technique. It's about showing up and doing it consistently, even when you're exhausted, even when progress feels invisible. The days I was too worn down to do a thorough job were the days things slipped backward. That's not a failure of willpower. It's the reality of what sustained wound management demands, and it's exactly why a care environment with dedicated staff can succeed where even the most devoted family caregiver eventually runs out of capacity.
A senior living community with trained nursing staff can provide what home settings often can't: daily wound assessment, daily dressing changes, properly applied compression that stays in place, and immediate response when something changes. The staff sees the wound every single day, which means they catch early signs of infection or deterioration before they become serious problems. They can ensure your parent's leg stays elevated during rest, monitor nutrition (which directly affects healing), and coordinate with wound care specialists or vascular surgeons when needed. That daily consistency is what separates a wound that heals from one that lingers for years.
Signs that a venous ulcer is improving include a shrinking wound bed, healthy pink granulation tissue replacing the yellow fibrin layer, reduced swelling in the surrounding skin, and less drainage. Signs of deterioration include increasing wound size, new areas of redness spreading outward from the wound edge, a foul odor, increased or discolored drainage, increasing pain, and any fever or chills. Families should understand these indicators so they can track progress and recognize when a change in care level is needed.
What Families Often Underestimate About Venous Ulcer Healing Timelines
One of the hardest conversations around venous leg ulcers is about time. Families often assume that once their parent is in a care community with daily wound management, the ulcer will heal within a few weeks. The reality is very different. Even with perfect compression therapy and daily dressing changes, research from the NHS and multiple clinical studies shows that most venous leg ulcers take three to six months to heal. Larger ulcers or those that have been open for more than a year can take significantly longer, and some may require advanced interventions like skin grafting or vascular surgery.
A study in the Journal of Vascular Surgery found that the healing rate at 26 weeks with consistent compression therapy was about 50%, rising to roughly 87% by 52 weeks. That means even with proper treatment, about half of venous ulcers are still open after six months. This isn't a sign that treatment is failing. It's the nature of the condition. Venous insufficiency is a chronic circulatory problem, and the tissue repair process in older adults is slower to begin with. Factors like diabetes, obesity, limited mobility, and poor nutrition can slow things down further. Larger wounds and those that have been open for more than a year face even steeper odds, with one study showing a 78% chance of healing failure at six months for ulcers older than a year and larger than 10 square centimeters. Setting realistic expectations upfront helps families avoid discouragement and premature decisions about changing care plans.
Ask the care team for measurable benchmarks. A wound that shrinks by 30% to 40% in the first four weeks of proper compression therapy is considered on track. If there's no measurable improvement after 12 weeks of consistent treatment, clinical guidelines recommend referral to a vascular specialist or wound care center for reassessment.
How Senior Living Communities Manage Chronic Wound Care
Not every senior living community is equipped to handle complex wound care, and that distinction matters. Assisted living communities typically have licensed nursing staff who can perform daily dressing changes and monitor wound status. Some communities employ or contract with certified wound care nurses who specialize in chronic wounds. Others rely on visiting home health services to supplement their in-house care, which can still be an improvement over the home setting because the community's daily nursing staff provides monitoring between specialized visits.
Skilled nursing facilities offer the highest level of wound care support, with registered nurses available around the clock and the ability to administer IV antibiotics, perform wound debridement, and manage complex multi-layer compression protocols. If your parent's wound is severely infected, very large, or complicated by other medical conditions like diabetes or peripheral artery disease, a skilled nursing level of care may be the right starting point. From my years working in hospitals, I've seen patients transferred between care levels when their wound needs changed, and that flexibility is something to ask about when evaluating communities.
Some communities also coordinate with outpatient wound care clinics, where your parent can receive specialized treatments like negative pressure therapy or bioengineered skin substitutes that aren't available in a residential setting. The community handles transportation, follows the wound clinic's care plan between visits, and communicates progress back to the specialist. This kind of team-based approach tends to produce better outcomes than any single provider working alone.
What to Ask When Evaluating a Senior Living Community for Wound Care
The questions you ask during tours and intake meetings will tell you more than any brochure. Start with the basics: Does the community have licensed nursing staff on-site daily, including weekends? How often are wounds assessed and dressings changed? Do they have staff trained specifically in compression bandaging, or do they rely entirely on outside wound care services? Ask about their protocol for recognizing and responding to wound infections. A community that can describe their escalation process, who they call, how quickly they respond, how they communicate changes to the family, is one that takes wound care seriously.
Ask whether the community has experience with venous leg ulcers specifically. Chronic wound management requires different skills than standard medication management or personal care assistance. You'll also want to know about their relationship with wound care specialists and vascular surgeons in the area. A community that already has referral relationships with local wound clinics can get your parent seen faster if the ulcer isn't responding to standard care. Don't hesitate to ask about staffing ratios on evenings and weekends, because wound complications don't wait for Monday mornings.
Nutrition is another factor that families overlook. Wound healing requires adequate protein, zinc, vitamin C, and overall caloric intake. Many older adults with chronic wounds are also malnourished, which slows healing even further. Ask the community whether they involve a dietitian in care planning for residents with chronic wounds, and whether meals can be adjusted to support tissue repair. A community that thinks about wound care holistically, not just the dressing itself, is more likely to produce results. During my time in the hospital system, the patients whose wounds healed best were almost always the ones with a coordinated care plan that included nutrition, mobility, and wound management working together.
Understanding the Costs of Chronic Wound Management in Senior Living
Chronic wound care adds a layer of cost that many families don't anticipate. The base monthly rate for assisted living typically covers room, meals, and a standard level of personal care assistance. Daily wound management, compression supplies, and specialized nursing time are often billed as additional care charges, sometimes called a "level of care" add-on. These can range from a few hundred to over a thousand dollars per month depending on the complexity of the wound and the frequency of dressing changes.
Research estimates that treating a single chronic venous ulcer costs between $1,100 and $2,800 per wound episode in direct medical expenses as of recent data, though total costs including home health visits, supplies, and specialist appointments often run much higher over the full healing period. Annual U.S. spending on venous leg ulcer treatment has been estimated at $15 billion. When our family faced the financial reality of professional care for a loved one, the numbers were a shock. But the cost of not treating the wound properly, repeated infections, emergency room visits, potential hospitalization, is almost always higher. Ask communities for a detailed breakdown of wound care charges before signing an agreement, and confirm what is included in the base rate versus what triggers additional fees.
Medicare may cover some wound care services if your parent qualifies for skilled nursing or home health benefits, but coverage varies by situation and care setting. If your parent is transitioning from a hospital stay, a short-term skilled nursing stay for wound care may be partially covered under Medicare Part A. It's worth speaking with the community's billing coordinator and your parent's Medicare plan to understand what out-of-pocket costs to expect.
Preventing Recurrence: Why Healing Isn't the Finish Line
Even after a venous leg ulcer heals, the underlying venous insufficiency doesn't go away. Recurrence rates for venous ulcers are high, with research showing that up to 70% of patients experience another ulcer if they don't continue preventive compression therapy. A 2024 Cochrane review confirmed that wearing compression stockings after healing reduces the risk of recurrence by roughly half. The key is consistency: stockings need to be worn daily, fitted properly, and replaced every three to six months as they lose their elasticity.
For older adults in a senior living community, this is actually one of the advantages of the care setting. Staff can help your parent put on and remove compression stockings each day, monitor the skin underneath for early warning signs, and ensure the stockings are replaced on schedule. At home, many seniors struggle to put on compression stockings independently because of limited grip strength, flexibility issues, or simply forgetting. That daily assistance alone can make the difference between a wound that stays healed and one that comes back within a year.
Beyond compression, ongoing prevention includes keeping the skin moisturized, maintaining gentle activity to support blood flow, elevating the legs during rest, and managing related conditions like obesity, diabetes, or high blood pressure. Having worked with elderly patients in hospital settings for years, I've noticed that the ones who maintain their mobility, even gentle walking, tend to have better circulation outcomes than those who become sedentary. A care community that encourages safe physical activity as part of the daily routine is supporting wound prevention whether they frame it that way or not.
Taking the Next Step With Confidence
Watching a wound on your parent's leg refuse to heal is exhausting and worrying, especially when you've already been doing everything you can at home. Venous leg ulcers are a medical condition that responds to consistent, knowledgeable care, and the right senior living environment can provide the daily wound management that changes outcomes. You're not giving up by seeking a higher level of support. You're getting your parent what the wound actually needs.
Start by talking with your parent's doctor or wound care specialist about what level of care the ulcer requires. Tour communities with specific wound care questions ready. Ask to speak with nursing staff directly, not just admissions coordinators, and trust your instincts about whether the team understands what your parent needs.
The fact that you're researching this means you're already advocating for your parent in the way that matters most. A wound that hasn't healed in months at home can heal in a setting where trained staff see it every single day. That consistency, that daily attention and proper compression, is what gives the tissue underneath a real chance to recover. Your parent deserves that chance, and you deserve the peace of mind that comes with knowing the care is handled right.