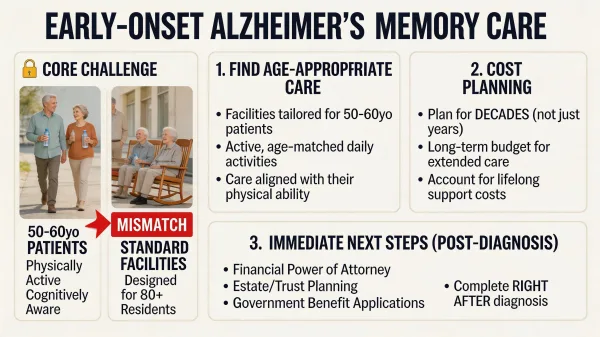
Most memory care facilities in the United States are built for people in their late 70s and 80s. The activities are gentle, the pace is slow, and the common areas are quiet. And when your parent is diagnosed with early-onset Alzheimer's at 55 or 58 or 62, you quickly realize that almost nothing about the standard memory care model fits the person you're trying to help.
Early stage Alzheimer's memory care for younger patients is one of the hardest searches a family can face, because the system wasn't designed with them in mind. Your parent may still be physically strong, still interested in hiking or cycling, still aware enough to feel out of place sitting in a circle with residents two decades older. The gap between what your parent needs and what most facilities offer is real, and it affects everything from daily quality of life to how fast cognitive decline progresses.
When a family member of mine was diagnosed with dementia, one of the first things that hit us was how completely unprepared the system was for someone who didn't fit the typical profile. The assumption that dementia is an old person's disease shaped every facility we visited, every brochure we picked up, every conversation we had with admissions coordinators. If your family is in this situation, you're not imagining the disconnect. It's there.
This article covers what makes early-onset Alzheimer's different, how to find memory care that actually fits a younger patient, the financial reality of paying for care that could stretch over a decade or more, and the legal and benefits steps you can't afford to put off.
What Makes Early-Onset Alzheimer's Different
Early-onset Alzheimer's (also called younger-onset Alzheimer's) is diagnosed in people under age 65. According to the Alzheimer's Association's 2025 Facts and Figures report, roughly 200,000 Americans under 65 are currently living with younger-onset dementia. That's a small fraction of the more than 7.2 million Americans 65 and older with Alzheimer's, which helps explain why the entire care infrastructure is built around older patients.
The clinical differences matter, too. Younger patients often present with symptoms that don't look like textbook Alzheimer's at first. Instead of gradual memory loss, early signs may include difficulty with complex tasks at work, problems finding words, personality changes, or trouble with spatial awareness. Misdiagnosis is common. Many younger patients spend years being treated for depression, stress, or burnout before anyone considers dementia. Research suggests the average diagnostic delay for younger-onset dementia is three to five years, longer than for late-onset cases.
The life-stage impact is what separates early-onset from late-onset in ways that go far beyond medicine. A 58-year-old diagnosed with Alzheimer's may still have a mortgage, a job, a spouse who works, and adult children who are just starting their own careers. The diagnosis doesn't just change the patient's life. It restructures the entire family's finances, roles, and future plans in one conversation.
Families dealing with early-onset also face a longer disease trajectory. While the average survival after an Alzheimer's diagnosis is four to eight years for someone diagnosed at 75, younger patients who are otherwise physically healthy may live with the disease for 8 to 12 years or longer. That extended timeline affects every decision, from the type of care facility you choose to how you structure financial planning.
Why Standard Memory Care Falls Short for Younger Patients
Walk into most memory care communities and you'll see programming designed for residents with limited mobility and advanced cognitive decline: chair exercises, simple crafts, music from the 1940s. For an 85-year-old with late-stage dementia, this can be appropriate and comforting. For a 58-year-old who was running 5Ks six months ago, it's a mismatch that families notice immediately.
In practice, this is where things break down. Many facilities will tell you they accept early-onset patients. Accepting someone and actually having programming designed for them are two very different things. A younger resident placed among people 20 to 25 years older, with significantly different physical abilities and interests, often withdraws. They stop participating and become isolated. And research consistently shows that social isolation and physical inactivity accelerate cognitive decline in dementia patients at every stage.
I've seen this pattern play out from the clinical side, too. Working in hospitals for nearly 20 years, I've watched how quickly patients decline when they're in environments that don't match their needs or abilities. The body and the brain are connected. When a physically capable person stops moving because nothing in their environment encourages movement, the decline compounds.
Finding Age-Appropriate Early Stage Alzheimer's Memory Care
This is the section that matters most if your family is actively searching for placement. Finding memory care for younger patients requires asking different questions than you would for an older relative, and being willing to look beyond the closest or most convenient option.
Programming and Activities
The single biggest differentiator between a facility that truly serves early-onset patients and one that simply admits them is programming. Look for communities that offer activities calibrated to higher cognitive and physical function. This might include structured outdoor walks or hiking groups, fitness programs beyond seated exercises, technology-based cognitive stimulation (tablets, interactive games, virtual reality programs), cooking or workshop activities that involve real skill use, and small-group outings to restaurants, parks, or cultural events. A younger patient with early to mid-stage Alzheimer's can often still engage with complex activities, carry on conversations, and participate in physical exercise that would be inappropriate for a frailer, older resident. Programming should reflect that.
Physical Activity Options
This deserves its own emphasis because it's so often overlooked. A 58-year-old with early-onset Alzheimer's may be in excellent physical health aside from their cognitive diagnosis. They need access to real exercise, not just a hallway to walk. Ask about gym equipment, outdoor spaces for walking or gardening, organized fitness classes, and whether the facility has staff trained to supervise physical activity for cognitively impaired but physically able residents. Physical exercise is one of the few interventions consistently shown to slow cognitive decline, and removing it from a younger patient's life because the facility isn't set up for it is a preventable loss.
Peer Grouping
Some larger memory care communities have begun creating separate programming tracks or even separate wings for younger residents or those in earlier stages of dementia. This is still uncommon, but it's worth asking about. A younger patient who can interact with peers closer to their own age and cognitive level will engage more, socialize more, and maintain function longer than one who is grouped with residents in much later stages of decline. If a facility doesn't offer formal peer grouping, ask how many current residents are under 70. If the answer is zero, that tells you something about whether your parent will find connection there.
Technology Integration
Younger patients are more likely to have been regular technology users before their diagnosis. Facilities that integrate tablets, video calling with family, music streaming personalized to the patient's preferences, and GPS-enabled wander management systems are better equipped for this population. Technology can also support cognitive engagement in ways that paper-based activities can't match for someone who spent decades using computers and smartphones.
Why Placement Fit Matters More Than You Think
Placing a 58-year-old in a facility designed for 85-year-olds doesn't just affect their daily happiness. It can accelerate decline. When a younger, more physically capable resident has no peers to interact with, no activities that challenge them appropriately, and no physical outlet, they lose ground faster. Families often describe watching their loved one "give up" after placement in an environment that doesn't fit. That's not a failure of willpower. It's a predictable outcome of an environment that doesn't match the patient's needs. During my family's search for dementia care, I saw this gap firsthand. The facilities that looked beautiful in brochures were often designed for a resident profile that didn't match our situation at all. Finding the right fit took longer and required looking farther than we expected.
The Financial Reality of Decades of Early-Onset Alzheimer's Care
Here is where early-onset Alzheimer's diverges most sharply from late-onset, and where families are often the least prepared. When someone is diagnosed at 78, the family is typically planning for two to four years of memory care. When someone is diagnosed at 58, the math changes completely.
As of 2025, the national median cost of memory care ranges roughly from $6,200 to $8,000 per month depending on the source and location, with significant variation by state. Urban areas and states with higher costs of living can push monthly rates above $10,000. At a midpoint of $7,000 per month, that's $84,000 per year. Memory care costs also typically increase 3% to 8% annually. For a patient diagnosed at 58 who may need care for 8 to 12 years, the total cost can reach $700,000 to well over $1 million, even before factoring in annual rate increases. That number is not designed to scare you, but families need to plan with realistic figures. Most families planning for late-onset care are working with a two-to-three-year horizon of $180,000 to $270,000. The early-onset timeline multiplies that by three or four. And because the patient is younger, they're often still carrying financial obligations that an 80-year-old wouldn't: a mortgage, car payments, possibly college tuition for their children. The household is losing a primary income at the same time it's taking on the largest expense the family has ever faced.
When our family faced a dementia diagnosis, the financial shock was one of the first things that knocked us sideways. We had no framework for what memory care would cost, no sense of how long we'd be paying, and no time to ease into the planning because the cognitive decline was moving faster than any of us expected. I remember sitting with the numbers and realizing that every week we delayed making financial decisions was a week we couldn't get back. That urgency doesn't show up in the brochures, but it's the reality that shapes everything else.
Long-Term Care Insurance
If your parent purchased a long-term care insurance policy before the diagnosis, it may cover a significant portion of memory care costs. Policies vary widely, but many cover $150 to $300 per day for a set number of years. Review the policy carefully for benefit triggers (typically the inability to perform two or more activities of daily living), daily or monthly caps, elimination periods (the waiting period before benefits start), and maximum lifetime payouts. If no policy exists, it's too late to purchase one after an Alzheimer's diagnosis. This is one of the most common financial regrets families report.
Social Security Disability Insurance (SSDI)
Early-onset Alzheimer's qualifies for expedited processing under the Social Security Administration's Compassionate Allowances program. This means faster access to SSDI benefits, with some claims processed in as little as 19 days compared to the typical wait of seven months or more. File as soon as the diagnosis is confirmed and work becomes unsustainable. Don't wait.
When filing, use the term "early-onset Alzheimer's" specifically. That's the language the SSA uses for its Compassionate Allowances list, and using the right terminology helps your claim get routed correctly. You'll need clinical records documenting progressive dementia from a neurologist or psychiatrist, and a daily living report filled out by a caregiver or family member. There's a mandatory five-month waiting period after the disability onset date before SSDI payments begin, and Medicare eligibility doesn't start until 24 months after SSDI payments begin. That's a total gap of roughly 29 months between disability onset and Medicare coverage. During that gap, you'll need to rely on employer-provided insurance (COBRA extends coverage up to 29 months for disabled workers), a spouse's plan, or marketplace coverage.
Spousal Financial Protection
If your parent is married, protecting the healthy spouse's financial future is critical. Medicaid, if it becomes necessary, has spousal impoverishment protections that allow the healthy spouse to keep a certain amount of assets and income. But Medicaid eligibility rules are complex and vary by state. An elder law attorney can help structure assets before they're spent down. This isn't about hiding money. It's about using legal protections that exist specifically for this situation.
Estate Planning Urgency
The window for legal and financial planning is shorter than most families realize. While the patient can still participate in decisions and sign legal documents, the family needs to establish or update a durable power of attorney, healthcare power of attorney and advance directives, review and update beneficiary designations on all accounts, and address any business ownership or partnership agreements. Once cognitive decline progresses past a certain point, the patient may no longer have the legal capacity to sign documents. Every month you delay narrows the window.
Benefits, Insurance, and the Timeline You Can't Ignore
Consider a situation where a 58-year-old father is diagnosed with early-onset Alzheimer's while still employed. His 30-year-old daughter is suddenly the one researching care options, calling facilities, and trying to figure out his disability benefits, all while he still seems mostly like himself on good days. Every memory care facility she tours is filled with residents 20 years older than her dad. His mortgage isn't paid off. His employer needs to know what's happening. And the clock on his ability to participate in his own legal and financial planning is already ticking.
This is not a hypothetical edge case. This is the reality for thousands of families every year. And the timeline for action is tighter than families expect.
The priority list for the first 90 days after diagnosis should include filing for SSDI (use the term "early-onset Alzheimer's" specifically when filing), consulting an elder law attorney about power of attorney and asset protection, reviewing all insurance policies (health, life, long-term care, disability), notifying the employer and understanding short-term and long-term disability options through work, and beginning the memory care research process, even if placement isn't needed yet. Starting early gives you options. Waiting until a crisis forces placement takes most of those options away.
The Emotional Weight on Younger Families
The grief that comes with early-onset Alzheimer's is different. It arrives decades before anyone expected it. The adult child processing this diagnosis may be in their late 20s or early 30s, still figuring out their own life, suddenly facing a caregiving role they assumed was 20 years away. Some are planning weddings their parent may not fully remember. Others are having children their parent may not recognize in a few years.
Spouses face a different version of the same devastation. A healthy 55-year-old who expected to grow old with their partner is instead becoming a full-time caregiver, managing medications, handling finances alone, and watching the person they married disappear slowly. The romantic partnership shifts into a caregiving relationship, and that transition carries a kind of grief that doesn't have a clean name. From my years as a caregiver for a terminally ill spouse, I can tell you that the loneliness of watching someone you love change in front of you is something the people around you rarely understand.
If there are younger children in the home, the family is dealing with an added layer of complexity. A teenager watching a parent lose cognitive function processes that differently than an adult child. They may not have the maturity to separate the disease from the person, and they may not want to talk about it with peers. Family counseling that includes age-appropriate conversations about dementia can prevent long-term emotional damage for kids who are watching something they can't fully make sense of.
Support groups specifically for early-onset families exist through the Alzheimer's Association and local chapters. Connecting with other families in the same situation is one of the most valuable things you can do, because the isolation of a diagnosis no one your age is dealing with is its own burden. You are not the only family going through this.
Questions to Ask When Touring Memory Care for a Younger Patient
Not all memory care facilities will be transparent about their limitations. These questions are designed to reveal whether a community can actually serve a younger, more physically active resident or whether they're simply willing to take the admission.
How many residents are currently under age 70? What does a typical day look like for your most physically active residents? Do you offer fitness programs or physical activities beyond chair exercises? Is there outdoor space residents can access safely? How do you handle programming for residents at different stages of cognitive decline? Do you have experience with early-onset Alzheimer's patients specifically? What technology do residents have access to? Can residents maintain any level of independence in daily routines? How do you approach the transition when a younger resident needs to move to a higher level of care?
Pay attention to what you see during the tour, not just what you hear. Are residents engaged, or are they sitting in front of a television? Is the common area quiet at 10 a.m. on a Tuesday, or is there actual activity happening? Do staff members interact with residents by name, or do they move through the hallways without stopping? From visiting care facilities during my years doing mobile X-ray work, I learned that the gap between what a facility says in its marketing and what actually happens inside can be significant. Trust what you observe over what you're told.
If the admissions coordinator can't answer these questions with specifics, or if the answers suggest that all residents follow the same programming regardless of age or ability, keep looking. Tour at least three to five communities before making a decision, and visit your top choices more than once, at different times of day. The right fit is worth the search.
Finding Your Way Forward
Early-onset Alzheimer's asks more of families than almost any other diagnosis. It asks you to plan for a future that may stretch a decade or longer. It asks you to find care in a system that wasn't built for your situation. And it asks you to make financial and legal decisions under pressure, often before you feel ready.
But the families who start early, who research thoroughly, and who ask hard questions of every facility they visit are the ones who find better outcomes. The right memory care placement exists. It may take more time and more phone calls to find it, but a facility where your parent is physically active, socially connected, and cared for by staff who understand younger-onset dementia will make a measurable difference in their quality of life and the pace of their decline.
Start the search before you need to. Talk to an elder law attorney this month, not next year. File for SSDI the moment work becomes unsustainable. Connect with the Alzheimer's Association's early-onset support programs so you're not doing this alone. And know that the fact you're researching this right now, even though it's hard, means you're already doing right by your parent.