This article is for informational purposes only and does not constitute medical, psychiatric, or legal advice. Conditions like PTSD and dementia require evaluation and ongoing care from qualified healthcare providers. VA benefit amounts, eligibility rules, and program availability change over time. Confirm current details with the VA or an accredited Veterans Service Officer before making financial or care decisions.
The first nightmare in thirty years is usually what tells a family something has changed. A Vietnam veteran who's been stable for decades suddenly wakes up shouting, and a wife who hasn't seen her husband like this since the 1980s calls her adult daughter the next morning, scared. By the time the family connects the dots, they realize they aren't dealing with one condition. They're dealing with two.
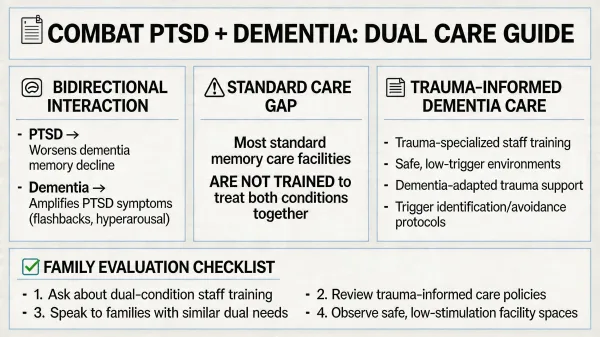
When combat PTSD and dementia overlap in an aging veteran, the care problem becomes something standard memory care facilities often aren't equipped to handle. Research shows PTSD is a significant independent risk factor for developing dementia, and cognitive decline can reactivate PTSD symptoms dormant for decades. The two conditions can amplify each other, creating care needs generic memory care training wasn't designed around.
This guide is for families of veterans who carry combat PTSD into their later years and are now facing cognitive decline on top of it. It covers what the research says about how PTSD and dementia interact, why common dementia care approaches can harm trauma survivors, what trauma-informed dementia care looks like in practice, and how to evaluate whether a memory care community can genuinely handle both conditions or just markets itself as "veteran-friendly."
In the ER, I've seen what happens when a veteran with PTSD is confused and scared, and that experience is part of why I went deep on the research for this piece.
How Combat PTSD and Dementia Interact in Aging Veterans
Combat PTSD and dementia interact in both directions: long-standing PTSD appears to be an independent risk factor for later dementia, and cognitive decline can reactivate PTSD symptoms that have been dormant for decades. The combination often produces nightmares, paranoia, startle responses, aggression, and trauma re-experiencing that standard memory care approaches may unintentionally worsen.
PTSD as an Independent Risk Factor for Dementia
A 2020 systematic review and meta-analysis in the British Journal of Psychiatry pooled data from longitudinal studies covering more than 1.6 million people and found PTSD was associated with roughly a 61 percent increased risk of all-cause dementia in veteran populations and roughly a doubled risk in general populations. The pattern held up even after adjusting for depression, substance use, and traumatic brain injury. A 2010 VA cohort study of 181,000 older veterans published in JAMA Psychiatry reached a similar conclusion, finding those with PTSD were more than twice as likely to develop dementia during follow-up across every dementia subtype examined. The research doesn't prove PTSD directly causes dementia, but it consistently shows a strong association that doesn't disappear when other risk factors are controlled for. Proposed mechanisms include chronic stress hormone exposure, hippocampal volume changes, accelerated cellular aging, and cardiovascular effects that compound over decades. For a Vietnam veteran who has carried PTSD since 1968, that's fifty-plus years of biological wear on the same brain regions most affected by Alzheimer's and vascular dementia.
How Dementia Can Reactivate Dormant PTSD
The reverse direction matters just as much, because many combat veterans spent decades managing their PTSD through routine, control, avoidance of triggers, and the daily psychological effort of keeping the past in the past. Dementia strips away exactly the cognitive tools that made that management possible. As short-term memory fades, older memories often surface more vividly, emotional regulation weakens, and environmental cues that were filtered out for years suddenly land with full force. A 2022 qualitative study of veterans in long-term care documented war-related nightmares, paranoia toward caregivers, aggression, and re-experiencing of military trauma as common features when PTSD symptoms and dementia co-occur. Prevalence estimates of PTSD among people with dementia run between roughly 4.7 and 7.8 percent in veteran studies, and the real number is likely higher because many older veterans never received a formal diagnosis.
Why Reality Orientation Can Make Things Worse
Older dementia care models often used reality orientation, the practice of correcting a person's confused statements with present-day facts. For a veteran whose brain is pulling up a 1969 firefight, being told "No, that's not happening, you're in Ohio in 2026" can feel dismissive at best and threatening at worst. Trauma survivors re-experiencing combat memories need the care team to respond to the emotion, not argue with the content. Trauma-informed dementia care means validating the feeling, reducing triggering stimuli, and redirecting gently, rather than insisting the veteran accept a reality his brain can't currently access.
Where This Gets Hard: Most Memory Care Isn't Trauma-Informed
Here's the part families often don't learn until there's been a triggering incident: the majority of standard memory care facilities don't train their staff in trauma-informed care. Most training focuses on dementia behaviors in general, not on how those behaviors present differently when the resident has combat trauma layered underneath. Staff learn redirection techniques for a resident who thinks it's 1985, but they often don't learn what to do when a resident thinks it's 1968 and the person approaching his bed is a threat. Families usually find out about this gap the hard way. A well-meaning aide tries to wake a veteran by touching his shoulder and he swings. A shower feels like a forced restraint, or a locked memory care door reads as capture. These aren't failures of the veteran. They're failures of a care model built around generic dementia rather than trauma-informed dementia.
I'll be direct about what this looks like from the inside. I've cared for elderly veterans in the ER who came in for something routine, a fall or a urinary tract infection, whose confusion pulled decades of combat right to the surface. The fluorescent lights, the noise, the sense of being restrained by monitors and IV lines, all of it can reactivate trauma a family thought was long settled. When those same men land in a memory care facility that isn't trauma-informed, the same cascade plays out every day. The hardest conversation with a family isn't that their father is declining faster than expected. It's that the environment is fighting him.
Symptoms Families Notice When PTSD and Dementia Collide
The overlap usually shows up in a few recognizable patterns. Nightmares that stopped decades ago return and become frequent, hypervigilance that used to be manageable becomes constant, and a veteran who was gentle becomes suspicious of familiar family members. Confusion about time and place pulls him back into specific combat memories rather than generic disorientation. Consider a situation where your father, who served in Korea or Vietnam, has been stable for years and is now in early-stage Alzheimer's. He starts sleeping with a light on for the first time in his adult life, he asks where his weapon is, he won't sit with his back to a door, and he becomes combative when an aide enters his room at night. These aren't new personality changes. They're old trauma responses surfacing through the openings dementia is creating. Not every aging veteran with dementia experiences this pattern, but for those who do, signs usually appear within the first year of noticeable cognitive decline and worsen unless the environment adapts.
Finding a Memory Care Community That Can Handle Both
A "veteran-friendly" label is marketing, not accreditation, and any community can use it. What you actually need to evaluate is whether staff are trained to handle trauma responses in a dementia context, not whether the lobby has a flag or the admissions brochure mentions Aid and Attendance.
Staff Training Questions to Ask
Ask directly what trauma-informed dementia care training the direct care staff have received, who provided it, and how often it's refreshed. Ask what they do when a resident has a nightmare, whether they enter the room in low light, and whether they approach from the front or from behind. Ask how they handle bathing and dressing resistance, because these are frequent trigger points for veterans with combat histories involving captivity, injury, or loss of control. A community that can handle both will answer with specifics, while a community that can't will answer with reassurances about how "we treat everyone with dignity." That kind of answer is a red flag rather than a real response.
Environmental Red Flags for Trauma Survivors
Look carefully at the physical environment, because loud overhead paging, sudden fire alarm tests without notification, hallways where staff can come up behind residents, and memory care units that feel like lockdown rather than residential can all escalate a veteran with PTSD. Ask about the noise level at shift change, whether rooms can be arranged so the bed faces the door, and whether the veteran can have a personal item placed within view from bed. Small adjustments like these prevent triggering incidents that would otherwise get written off as "agitation."
Medication and Behavioral Approaches
Ask how the community and its medical director approach behavioral symptoms. Over-reliance on antipsychotics to manage PTSD-driven dementia behaviors is common and problematic. Trauma-informed communities work with a geriatric psychiatrist who understands veteran-specific care and can distinguish between dementia agitation that responds to environmental intervention and PTSD re-experiencing that needs a different approach. Ask whether the facility partners with the VA for mental health consultation, whether the medical director has experience with older veterans specifically, and what the facility's antipsychotic use rate looks like compared to state averages.
How to Verify "Veteran-Friendly" Is Real
Request a tour during dinner or late evening rather than morning, because that's when sundowning and trauma symptoms tend to intensify. Watch how staff interact with current residents who are agitated, and ask to speak with one or two families of veterans currently living there. If admissions can't or won't arrange that conversation, assume the "veteran-friendly" label is marketing and keep looking.
What Trauma-Informed Dementia Care Looks Like Day to Day
Trauma-informed care is built on six principles the Substance Abuse and Mental Health Services Administration (SAMHSA) identifies for any trauma-informed approach: safety, trustworthiness and transparency, peer support, collaboration and mutuality, empowerment and choice, and cultural and historical awareness. In a memory care setting, those principles translate into specific daily practices. Staff learn the veteran's service history from the family at intake, including what topics to avoid and what might trigger him. Care routines are predictable and announced before they happen, aides don't enter rooms silently at night, and showers are offered with warning and with choice about water temperature and timing. Exit doors aren't described as locked but as "the way out for later." When a resident has a flashback, staff respond to the feeling of fear rather than arguing with the content. The shift SAMHSA describes, from "what's wrong with you" to "what happened to you," is the heart of the approach, and it requires staff trained in both dementia and trauma.
VA Benefits That Can Help Pay for Veteran Memory Care
The VA offers several programs that can offset memory care costs for eligible veterans, though none directly cover the room and board portion of private memory care. The Aid and Attendance pension is an enhanced monthly pension for wartime veterans who need help with activities of daily living. For the benefit year running December 2025 through November 2026, the Maximum Annual Pension Rate with Aid and Attendance was approximately $28,296 for a single veteran (about $2,358 per month) and $33,548 for a veteran with a dependent spouse (about $2,796 per month), according to VA pension rate tables. Actual payments are reduced by countable income, and unreimbursed medical expenses above 5 percent of the MAPR can be deducted to increase the benefit. Aid and Attendance doesn't cover the full cost of memory care in most markets, which commonly runs $6,000 to $8,000 or more per month as of 2025, but it can close a meaningful portion of the gap.
VA Community Living Centers (CLCs) provide long-term care including dementia care for enrolled veterans, and some have specialized PTSD and dementia programming, but wait times can be long and eligibility generally favors veterans with higher service-connected disability ratings. The VA Caregiver Support Program offers education, training, and respite for family caregivers. A local Veterans Service Officer (VSO) can help families apply for benefits at no cost and is almost always a better starting point than a paid claims service.
How Families Can Help Before and During the Transition
Before placement is decided, document your veteran's service history in enough detail that future care staff can interpret his symptoms. Branch of service, era, deployment locations, injuries, known trigger topics, and any trauma he has disclosed over the years all belong in a one-page document the family can share with the facility. Many veterans never told their spouses or children the details, so the document may need to focus on what you do know and what to avoid.
Build the daily environment around predictability by reducing loud startle sources, announcing who's entering a room before stepping in, and not arguing with confused statements that carry trauma content. When your father insists someone's outside, skip the debate about whether it's true. Reassure him, check the door, and sit with him until the fear passes. These are the same skills trauma-informed staff use in a memory care setting, and families can start using them at home well before placement becomes necessary. Start early on the logistics, and begin the VA benefits application as soon as you suspect long-term care is coming, because approval timelines can run months.
Questions Families Often Ask
Does my father need to be diagnosed with PTSD for trauma-informed care to matter?
No formal diagnosis is required, and many older veterans never received one. Some managed their symptoms for decades without telling anyone. If your father is a combat veteran, assume the possibility of trauma and plan accordingly, because care staff can use trauma-informed approaches preventively without a formal diagnosis in the chart.
Is a VA Community Living Center better than a private memory care community?
It depends on availability and fit, and neither option is universally better. VA CLCs have experience with veterans and can be excellent, but availability is limited, wait times vary significantly by region, and quality isn't uniform across facilities. Private memory care that's truly trauma-informed can be a better option for some families, especially if location matters or wait times for the local CLC are long. Ask the VA social worker for an honest assessment of your options.
Should we tell my father he has dementia?
Early on, when he can still process it, most clinicians recommend honest conversation so he can participate in decisions about his own future. As the disease progresses and insight fades, repeated confrontation with the diagnosis tends to cause distress without changing anything. Trauma-informed care generally emphasizes meeting the person where he is rather than forcing recognition of a reality his brain can no longer access.
Can PTSD treatment still help at this stage?
Some evidence suggests PTSD treatment adapted for cognitive impairment can reduce symptoms even in people with dementia, though the research is still early and limited. Ask a VA geriatric psychiatrist or your father's primary care team what options exist for his specific stage of cognitive function and what realistic benefit looks like.
Bringing It Together
Combat PTSD and dementia in an aging veteran is a specific kind of care problem, not a generic one. The research is clear that the two conditions interact, and the clinical reality is that most standard memory care facilities haven't trained their staff to handle the combination. That doesn't mean good care is unavailable. It means finding it takes more than checking for a flag in the lobby, and it takes asking questions most admissions teams aren't prepared to answer.
The families who do this well share a few habits. They document the veteran's service history early, they ask memory care communities specific questions about trauma-informed training and accept specific answers only, they start VA benefits applications well before they're needed, and they adjust the home environment to reduce triggers during placement decisions. They also accept that their father's behavior changes aren't personal but are the predictable result of two conditions interacting under a system that wasn't built with his history in mind. If you're reading this because something recent has made you realize you're dealing with both PTSD and dementia rather than dementia alone, you're in the right place. Take the research seriously, ask the hard questions, and remember that your father served and deserves care that sees all of him.