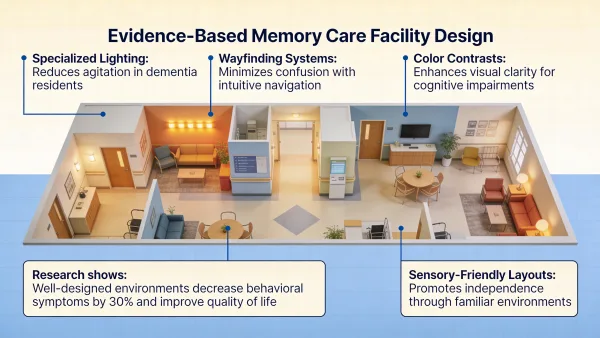
Research from the Journal of Housing for the Elderly found that residents in well-designed memory care facilities experience significantly lower levels of agitation compared to those in poorly designed spaces. The difference isn't subtle. We're talking about measurable reductions in behavioral symptoms, fewer falls, better sleep patterns, and less reliance on medication to manage distress.
This isn't about making places look nicer. It's about understanding how dementia changes the way people process their environment and then building spaces that work with those changes instead of against them.
When someone has Alzheimer's disease or another form of dementia, their brain struggles to interpret visual information, maintain spatial orientation, and filter sensory input. A hallway that seems straightforward to you might appear as a confusing maze of identical doors to someone with cognitive impairment. A shiny floor might look like water they're afraid to walk across. Fluorescent lights flickering at frequencies you don't consciously notice can trigger genuine distress.
Memory care design addresses these challenges through specific, research-backed architectural and interior choices. Every decision, from ceiling height to door color to where windows are placed, affects how residents experience their daily lives.
Evidence-Based Design Elements That Actually Work
The term "evidence-based design" gets thrown around a lot in senior living marketing, but what does it really mean? It means specific design choices backed by research showing measurable improvements in resident outcomes. Not guesses. Not trends. Actual data.
Lighting Systems That Support Circadian Rhythms
Dementia disrupts the body's internal clock, leading to the phenomenon caregivers call "sundowning," where confusion and agitation worsen in late afternoon and evening. Proper lighting helps reset these disrupted rhythms.
The Lighting Research Center found that seniors need approximately 70% more light than younger adults to see objects clearly. But it's not just about brightness. Modern memory care facilities use dynamic lighting systems that change throughout the day to mimic natural sunlight patterns. Morning light is brighter and bluer, supporting alertness. Evening light gradually shifts to warmer, dimmer tones, promoting natural sleep.
Research shows residents exposed to appropriate lighting sleep better at night, experience fewer episodes of agitation, and maintain better mood stability. Some facilities install light therapy boxes in common areas or use specialized ceiling fixtures that deliver therapeutic light doses without residents needing to do anything differently.
Lighting also affects safety. LED strips installed under beds help residents navigate bathroom trips at night without harsh overhead lights that fully wake them. Under-mirror lighting improves visibility for grooming without creating the glare that confuses many people with dementia.
Wayfinding Systems Built on Visual Processing
Up to 60% of people living with dementia will experience wandering at some point, according to the Alzheimer's Association. This isn't aimless movement. It's often a person trying to reach somewhere they think they need to be, but they can't figure out how to get there.
Effective wayfinding in memory care doesn't rely on residents reading signs or remembering directions. It uses visual cues that bypass the damaged parts of cognitive function and tap into deeper recognition systems.
Color-coded zones work when implemented correctly. Not just painting doors different colors, but creating entire color environments where the dining room area is consistently warm tones and the resident room corridors use cooler blues or greens. The color becomes associated with the function, reducing the need to read and process signs.
High-contrast elements help residents distinguish between different surfaces and objects. Doorframes painted in contrast to walls make openings obvious. Toilet seats in a different color than the bathroom floor prevent the "white on white" effect where everything blends together. Table settings with plates that contrast with placemats help residents see their food more clearly, which actually increases how much they eat.
Landmarks provide recognizable reference points. A distinctive piece of furniture, a large plant, or themed artwork creates visual anchors. Residents might not remember "turn left at the third door," but they can recognize "the hallway with the big fish tank" and know their room is nearby.
Memory boxes mounted outside resident rooms work better than names on doors. A shadow box containing personal items, family photos, and familiar objects creates instant recognition. The resident sees their grandson's baseball mitt or their mother's china teacup and knows "that's my space" without having to read or remember a room number.
Continuous loop designs prevent dead ends. When hallways circle back to starting points rather than terminating in walls, wandering residents can walk as much as they need without encountering frustrating barriers that increase agitation. They always end up somewhere they recognize.
Controlling Sensory Input
Dementia makes it harder to filter background noise and visual clutter. Things that neurotypical people tune out automatically become overwhelming. A TV playing in a common area, overhead announcements, multiple conversations, the hum of HVAC systems all layer into sensory chaos that manifests as anxiety and behavioral symptoms.
Memory care facilities use extensive acoustic treatment. Sound-absorbing materials in ceilings, carpet instead of hard flooring, and upholstered furniture all reduce noise bounce. They avoid overhead paging systems entirely. Staff use quiet communication devices. Some facilities play specifically selected ambient music at low volume to mask disruptive sounds without adding to confusion.
Visual simplification matters too. Busy patterns on carpets, wallpaper, or upholstery can trigger visual distortions. Some residents see patterns as obstacles or movement. Memory care design favors solid colors or very subtle patterns. Artwork is carefully chosen, avoiding abstracts that might be interpreted as threatening and favoring clear, recognizable images.
Glare causes serious problems. Windows need appropriate treatments that let in natural light without creating bright spots on floors that might look like puddles or holes. Matte finishes on floors and walls prevent light reflection. Glass-fronted artwork is avoided because the glare makes it impossible for many residents to see the actual image.
Spatial Layout That Reduces Confusion
The architecture itself matters as much as what you put in it. Studies on wayfinding behavior in people with dementia show they perform best in spaces with clear sight lines, minimal decision points, and predictable layouts.
Long double-loaded corridors (hallways with doors on both sides, like hotels) create the worst outcomes. Every door looks the same. There's no clear destination visible. Residents must make repeated decisions about which door might be theirs, leading to exhaustion and increased confusion.
Better designs use household models where 10-15 residents share a common living area with their private rooms clustered around it. The layout mimics a home, with a clear social center (like a family room and kitchen) and private spaces obviously connected to it. Residents can see from their doorway into the common area, providing constant orientation.
Room placement follows logic people with dementia can still grasp. Bathrooms connect directly to bedrooms through a private door, not out in a public hallway. Dining areas are near kitchens, not isolated. Activity spaces have windows with views to outdoor areas so residents can see what's happening before entering.
Safety Features That Don't Look Clinical
People with dementia lose depth perception and have trouble interpreting visual information. This creates serious fall risks, but institutional safety equipment often increases confusion and resistance.
Modern memory care design addresses this through thoughtful visual strategies. Flooring uses consistent colors throughout spaces to avoid the appearance of steps or holes where there are none. That black rubber threshold strip between rooms can look like a dangerous gap to someone with dementia.
Contrasting the first and last steps on staircases helps residents see where steps begin and end. But memory care facilities increasingly avoid stairs entirely, using ramps with gentle grades that feel like level walking.
Handrails extend the full length of hallways at appropriate heights, but they're designed to look like architectural details rather than medical equipment. Wood finishes, integration into wall design, and careful color choices make them feel less institutional.
Secure doors to exits or dangerous areas don't look locked. They might be camouflaged with murals that make the door blend into the wall. Or they might be painted the same color as the wall rather than a contrasting color that draws attention. The goal is reducing the urge to exit rather than physically preventing it, which causes less distress.
When Pretty Doesn't Equal Therapeutic
Here's where things break down in practice: facilities spend enormous amounts making spaces look beautiful for tour groups and families, but they miss the functional design elements that actually help residents with dementia.
You'll see communities with gorgeous lobbies, elegant furniture, and sophisticated color schemes that would photograph beautifully for marketing materials. Then you walk into the actual memory care neighborhood and find shiny floors creating glare, busy patterned wallpaper, low-contrast everything, and long institutional hallways.
The disconnect happens because designers focused on aesthetics instead of evidence. A stunning chandelier might be terrible for someone with dementia who perceives it as something falling from the ceiling. That beautiful abstract painting could be genuinely frightening to someone who can't process abstract images. The sleek, modern furniture with clean lines looks great but provides no visual cues about how to use it.
Good memory care design should look warm and residential, but that's a byproduct of getting the functional elements right, not the primary goal.
Layout Patterns That Support Independence
Memory care facilities use several tested layout models. The household model clusters 10-15 residents around a shared living area with a residential kitchen, dining space, and activities area. Each resident has a private room with bathroom connected to this common space. The model supports social connection while maintaining clear spatial orientation.
The neighborhood model groups multiple households together, creating small communities within the larger facility. Residents primarily stay within their neighborhood but can access shared amenities like therapy rooms or large gathering spaces.
Some facilities use the pavilion model with distinct buildings for different functions connected by covered walkways. This works well in areas with good weather and provides clear differentiation between sleeping areas, dining areas, and activity spaces.
Single-story designs outperform multi-story buildings for this population. Elevators confuse many residents, and the spatial disorientation of being on different floors increases behavioral symptoms.
Sensory Elements and Therapeutic Spaces
Research shows that appropriate sensory stimulation can reduce agitation when implemented carefully. Many facilities create multi-sensory rooms with controllable lighting, gentle sounds, tactile elements, and even aromatherapy options. These spaces provide calming interventions without medication.
Outdoor access matters significantly. Secured gardens with walking paths, raised planting beds, and seating areas give residents safe access to nature. Studies consistently show time outdoors reduces behavioral symptoms and improves sleep.
The gardens need specific design considerations. Paths should be obvious and lead somewhere clear rather than having multiple branches requiring decisions. Fencing should be attractive but secure, ideally using hedges or decorative elements rather than institutional chain link. Plants should be non-toxic since some residents will try to eat anything.
Some facilities create themed areas that tap into long-term memories. A 1950s-style room with period-appropriate furniture, music, and decor can help residents feel grounded. Others use familiar activities like folding laundry, setting a table, or organizing tools to provide purposeful engagement.
How Memory Care Design Supports Staff
Well-designed memory care doesn't just help residents. It reduces staff burden and improves care quality. Open sight lines from staff areas into common spaces let caregivers monitor multiple residents without intrusive surveillance. This increases response time and allows staff to intervene before situations escalate.
Proper acoustics mean staff can hear concerning sounds (like a fall or someone in distress) without constant background noise fatigue. Good lighting reduces strain during documentation and medication administration.
Decentralized care stations positioned within living areas rather than behind a central nurses station support the household model and keep staff embedded in resident life rather than separated behind a desk.
Aesthetics in Memory Care: Less Is Actually More
The aesthetic approach in memory care differs significantly from other senior living settings. Where independent living might embrace bold, trendy design, memory care succeeds through restraint and intentionality.
Colors should be familiar and residential. Earth tones, soft blues, gentle greens work well. Avoid trendy palettes that won't feel familiar to older adults. The goal is creating spaces that feel like the homes residents remember from their adult lives, typically mid-20th century residential styles.
Furniture should be recognizable in form and function. A clearly identifiable couch, armchair, and coffee table work better than modern furniture with ambiguous purpose. Residents need to see a chair and know it's for sitting without having to process unfamiliar design.
Artwork should be clear, representational, and pleasant. Landscapes, familiar animals, recognizable scenes. Avoid abstracts, dark or disturbing subjects, and anything that might be misinterpreted. Family photos throughout common spaces provide connection without the personalization issues of using actual resident photos (which can cause confusion when residents don't recognize themselves or deceased family members).
Decorative elements should serve dual purposes. That attractive wooden box isn't just decor; it holds activities supplies. The vintage radio isn't just nostalgic; it plays familiar music from the residents' young adult years. Everything should be both functional and familiar.
Questions to Ask About Memory Care Design
When evaluating memory care facilities, look past the marketing photos. Ask to spend time in the actual resident areas during normal daily activities. Observe whether the design elements actually work as intended.
Can residents see from their rooms into common areas? Are there clear sight lines to destinations like dining rooms? Is the lighting bright enough without harsh glare? How noisy is the environment during typical times?
Look at color contrast between floors and walls, doorframes and walls, toilet seats and floors. Check if residents' rooms have personalization options. Ask about wandering management and whether the facility uses camouflaged exits or visible locks (visible locks work against the goal).
Request information about the specific evidence-based design elements incorporated. Facilities serious about therapeutic design will have detailed answers about their lighting systems, wayfinding strategies, and acoustic treatments.
The Difference Design Makes
Memory care design won't stop dementia progression, but it significantly affects quality of life during that progression. Residents in well-designed facilities spend less time in distress, maintain independence longer, and require less medication for behavioral symptoms.
For families, this means visiting a parent who is calmer and more engaged. For staff, it means spending time on meaningful interaction rather than managing crisis after crisis created by poor design.
The best memory care design is invisible to residents. It simply makes their world make sense again, as much as that's possible. They can find their room. They can see their food. The space feels safe and familiar. They can move around without constant fear or confusion.
That's what therapeutic design actually means